
Thank you very much, Mr. Gut, I'm very happy to be here. It was very nice to meet so many people today who are interested in my book.And I hope to tell you something that I think is important.
I'm very happy to be here in China, because China, as you know, is in the middle of different kinds of revolutions. And I first came here about 30 years ago, and it is amazing to see how much China has become modern, and ultra-modern.
Today I was on the train, and it's so much nicer than our trains. So we have very much to learn from you, and now maybe I can try to tell you some things as well.
十分感谢你,热心肠先生,我很高兴来到这里。今天见到这么多对我的书感兴趣的人,真是太好了!我希望告诉大家一些我认为很重要的事情。
我很高兴来到中国,因为如大家所知,中国正处于各种各样的变革中。我第一次来这里是大约30年前,令人吃惊的是,现在中国已经成为如此现代化以及超现代化的国家。
今天我在火车上,发现中国的火车比美国的好很多,所以我们有很多东西要向你们学习,也许现在我也可以试着告诉大家一些事情。

So today I talk about our missing microbes.
And another way to look at this is that it's a story about ecology, about human ecology and how human ecology is changing.
I was lucky that I have a wonderful publisher, Hunan books, and they have submitted my book, Missing Microbes, and it just won a big award this year.
You can see that people all over the world are reading it, even in Chinese. And because it's being translated into a number of languages, and I'm very pleased that people in China will be able to read it.
为此今天我要讲讲关于“我们消失的微生物”的话题。
从另一种方式来看待的话,这是一个关于生态学、人体生态学与人体生态如何变化的故事。
很幸运我有一个很棒的出版商——湖南科技出版社,他们已经出版了我的书《消失的微生物》,并且它今年刚刚赢得了一个大奖。
在世界各地,你都能看到阅读这本书的人,包括中文版本,因为它被翻译成多种语言,我很高兴中国读者能读到这本书。

So now let me begin.
And I begin by showing these photographs of Greenland from outer space in 1992 and 2002.
And you can see that in 2002 there is less ice. And the reason that there's less ice is what we call global warming. And we can define global warming as a change in our macro-ecology because of human activities.
现在我要开始我的演讲。
我首先展示这些1992年和2002年从太空拍摄格陵兰岛的照片,大家可以看到2002年这里的冰川变少了,而冰变少的原因就是所说的全球变暖,我们可以把全球变暖定义为人类活动导致的宏观生态变化。
And what I'd like to talk about today is how our micro-ecology is changing because of human activities.
And unfortunately, I think it is happening on the same scale, and maybe even a little faster.
我今天要讲的是人类活动如何改变我们的微生态。
同样不幸的是,我觉得它发生的规模和全球变暖是相同的,甚至更快一些。
So I will begin by telling you some things about the United States, some things that many of you know already.
我首先要告诉大家一些关于美国的故事,是一些大多数人都已经知道的故事。
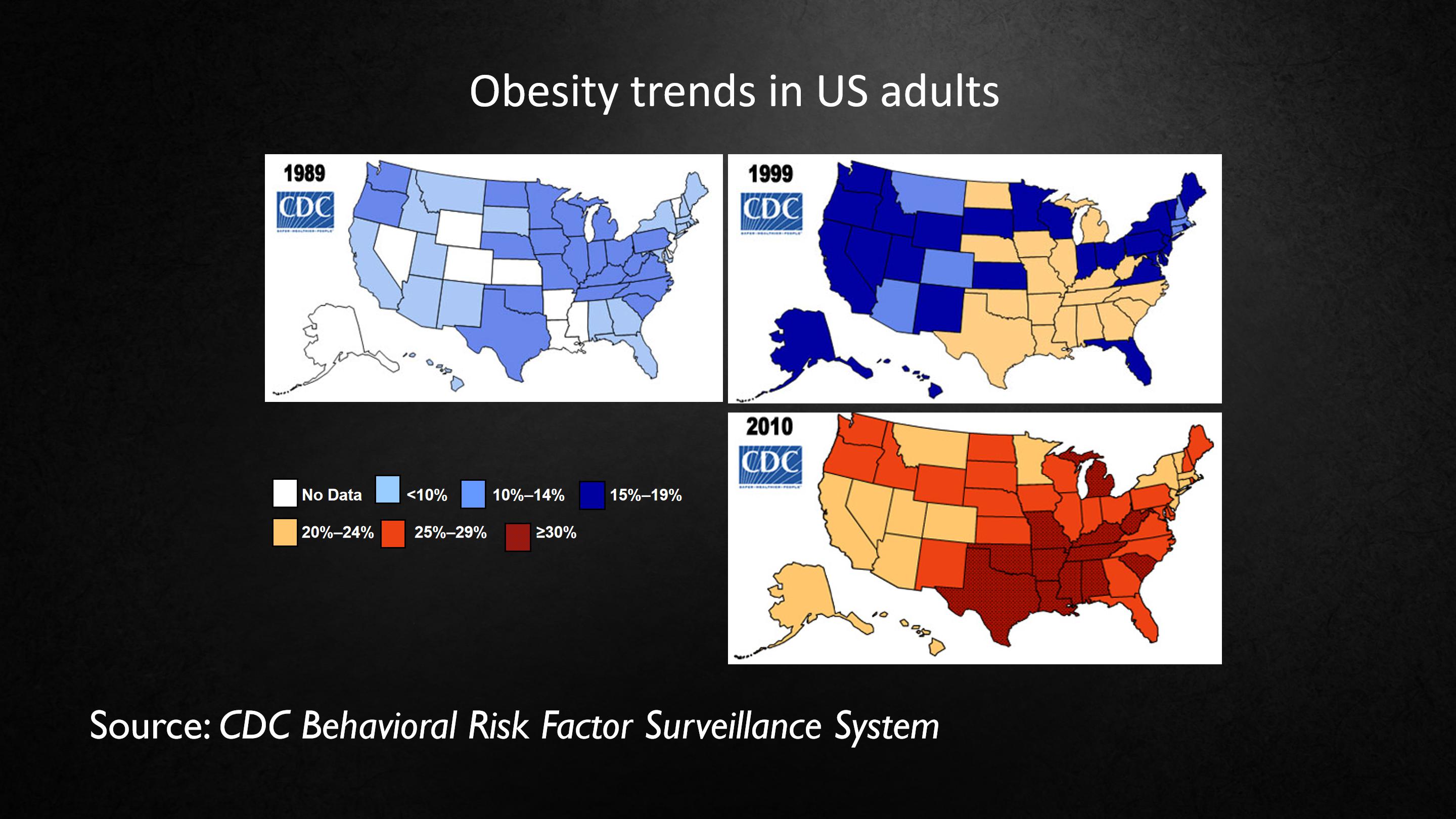
This slide behind me is about the trends in obesity in adults in the United States.
And there are three maps here. The first map is from 1989, and in that year there is no state in the United States where more than 14% of adults are obese. And the last map is from 2010, and at that time there is no state that has less than 20% obesity.
我身后这张幻灯片是关于美国成人肥胖的趋势图。
这里有三张地图,第一张地图是1989年,这时美国没有一个州的成年人肥胖率超过14%,最后一张地图是2010年,这时美国没有一个州的成年人肥胖率低于20%。
And so what's remarkable is that it's happening all over the country, and the difference between the first and the last map is only 21 years.
Something very powerful is happening.
因此值得注意的是,全美各地都是这样,第一张地图和最后一张地图之间仅相隔21年。
这个世界正在发生一些大事。
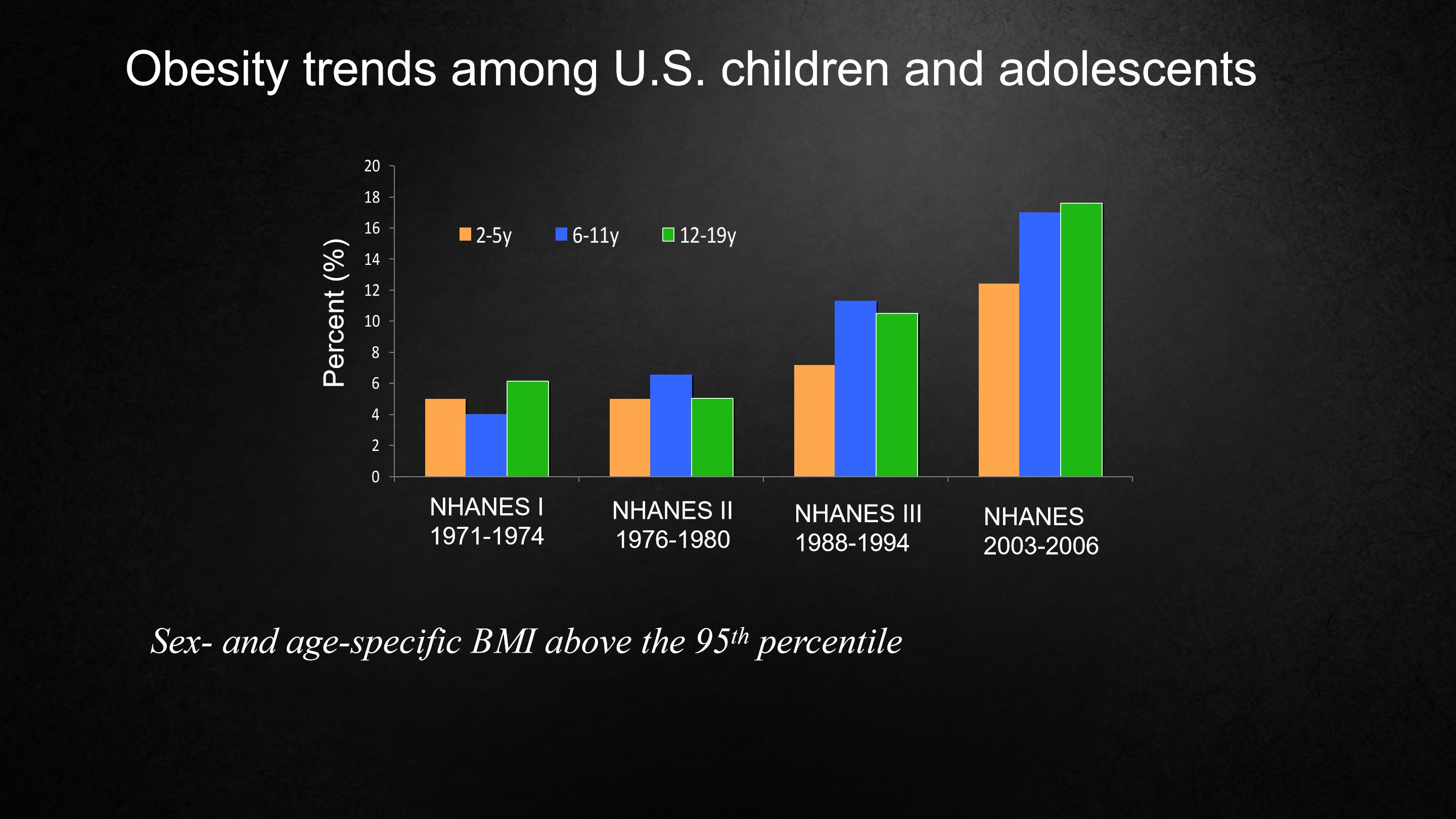
We know that obesity in adults begins in childhood.
And this is illustrated by this slide, looking at obesity trends over about a 35-year period. And you can see that over time, the trends are going up, even in the youngest children.
In fact, this is happening all over the world. And childhood obesity will one day lead to adult obesity.
我们知道成年人肥胖始于童年。
通过关注35年时间里的肥胖趋势,这张幻灯片说明了这一点,而且你们能发现随着时间的变迁,这一趋势仍在上升,甚至在儿童身上也是如此。
事实上,全世界都在发生这样的事情,童年的肥胖终有一天会导致成年人肥胖。
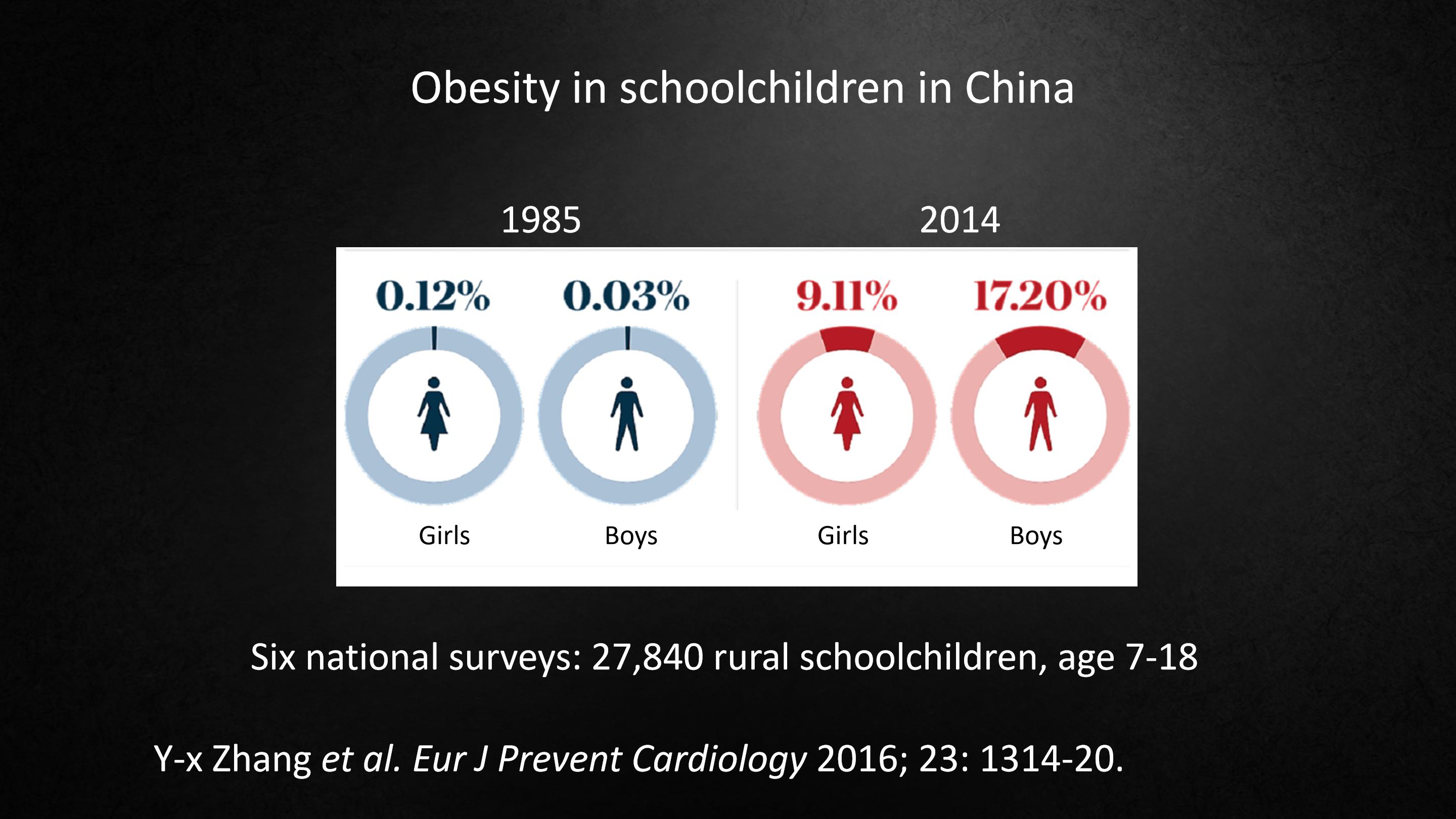
Now it is especially important to think about what's happening in China.
In 1985, there were very few children who were obese, and by 2014 the numbers have skyrocketed.
现在尤为重要的是想想中国正在发生什么?
在1985年,极少数的孩子会肥胖,但是在2014年,肥胖儿童的数字飙升。
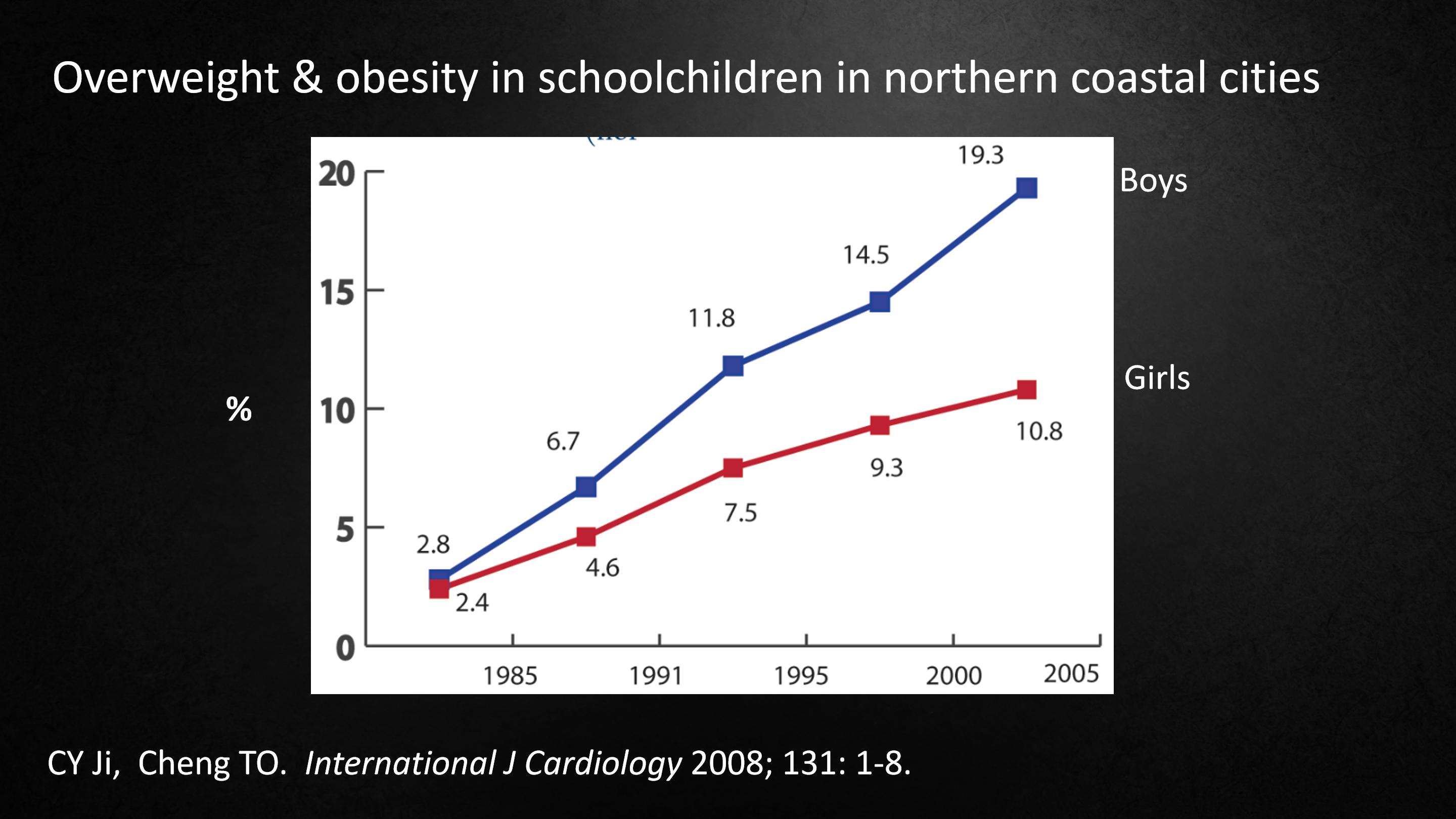
In fact, in boys in China, you're almost at the same rate as boys in the United States, and I think that's very bad news. And the trend shows no sign of getting any better.
实际上,中国男孩的肥胖率几乎和美国的差不多,我认为这是个坏消息,而且这种趋势没有任何好转的迹象。

Not just children. We're seeing it throughout our society, and I show this just to remind you.
In fact, it's happening to our pets, to our dogs and cats also. But obesity is not the only disease that is going up.
不仅仅是儿童,在整个社会人群中我们都能看到,我展示这些就是为了提醒大家。
其实,肥胖也会发生在我们的宠物,我们的狗和猫身上,但肥胖并不是唯一正在上升的疾病。
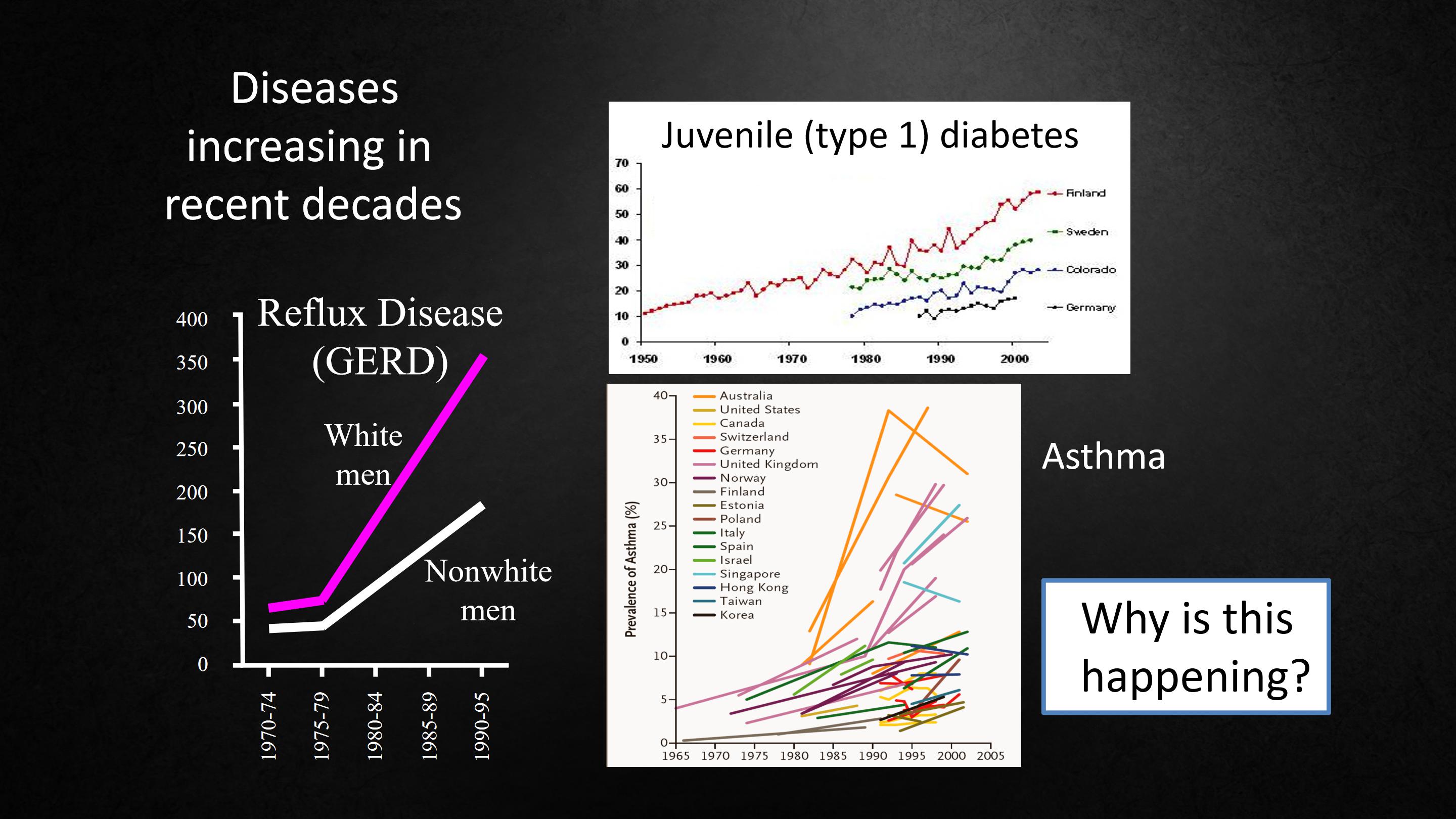
Now we see big rises in juvenile diabetes, type-1 diabetes. It's doubling every 20 or 25 years.
And asthma is going up everywhere. And diseases of the esophagus are rising dramatically.
And there are many others.
现在我们看到青少年糖尿病,即1型糖尿病的患病率也大幅上升,每20年或25年就会翻一番。
而且无论在哪里,哮喘患病率都在上升,食道疾病也正在急剧上升,还有很多其他疾病。
And the question is, why are all these diseases going up at the same time? Do they all have separate causes or is there one thing that is underlying all of them?
问题是,为什么所有这些疾病的患病率会同时上升?它们都有各自的原因吗?还是有一种原因潜伏其中?
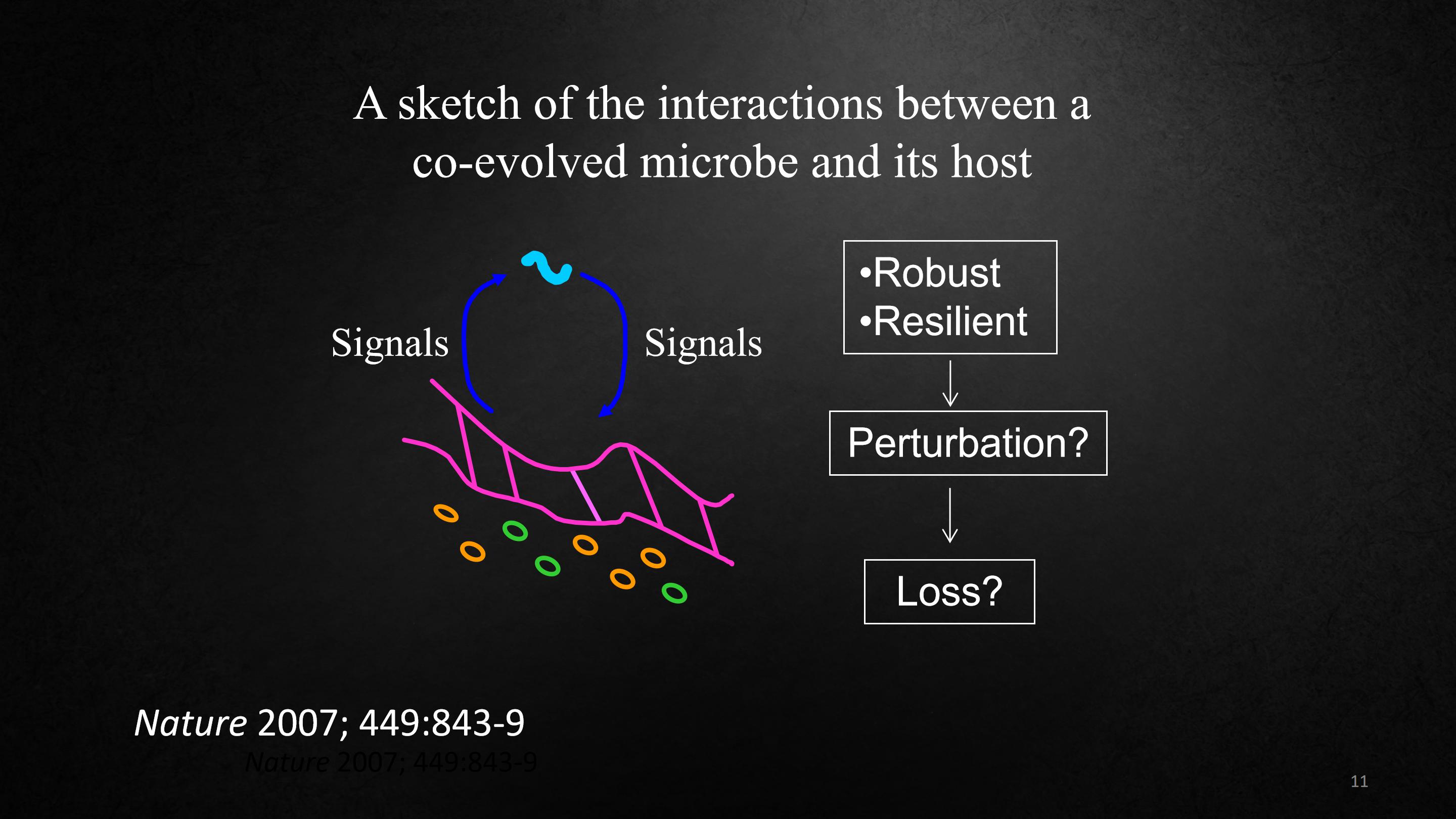
So in Missing Microbes, I talk about the idea that it's because of a change in our microbes, that it is underlying everything.
And that can be illustrated by this slide which is a sketch of the interactions between microbes that know our human biology.
所以在《消失的微生物》这本书中,我谈到了一个概念,认为这些是因为我们的微生物发生了变化,它是以上一切的潜在原因。
这可以用这张幻灯片来说明,它是了解我们人类生物学的微生物之间相互作用的示意图。
And this is from work I did with a mathematician, Denise Kirchner.
Our idea is that the microbes are talking to the cells of the human body and is receiving conversations back. And this forms an equilibrium.
And Denise has shown that this is a very strong equilibrium, it's robust, it's resilient.
这是我和数学家 Denise Kirchner 一起合作得到的成果。
我们的想法是微生物正在与人体细胞交流,并接受人体细胞的回话,这就形成了一种平衡。
Denise 已经表明这是一个很强大的平衡,它既稳健又有弹性。
What I want to talk about today is what happens when we lose that relationship? What happens when it's.. Firstly when it's disturbed? And then, ultimately, what happens when it's lost?
今天我想谈的是当我们失去这种关系时会发生什么?首先,当它被扰动时会发生什么?最后,当失去这种关系时会发生什么?
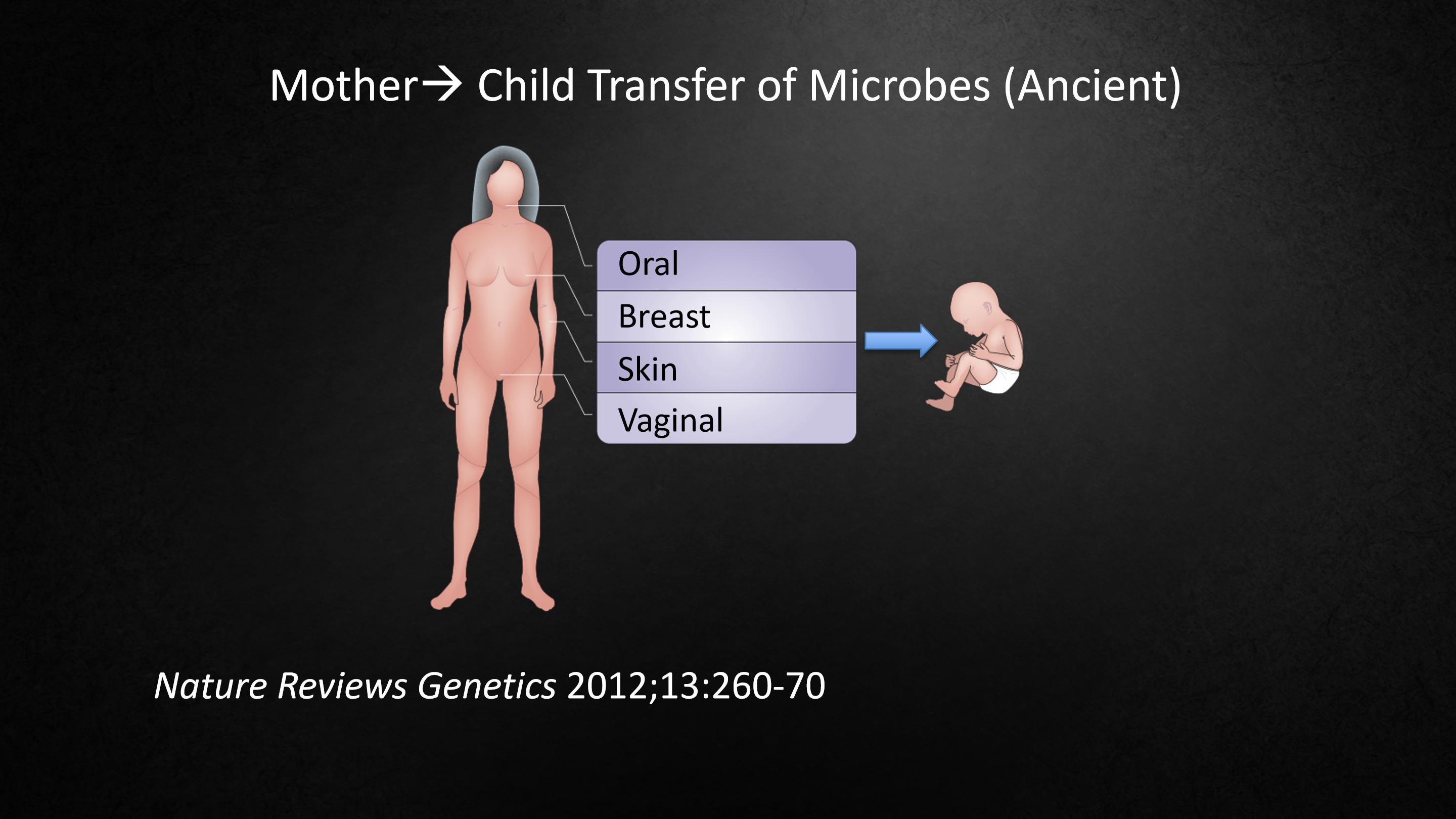
So to introduce the subject in another way, let me remind you that we humans are mammals.
And we begin our life in the womb, which is sterile.
Our big exposure to bacteria, to other microbes, happens when the water breaks, and the baby descends through the birth canal and is covered by the mom's microbes.
The baby swallows the microbes, and now they have contact with the mother's skin, with the mother's breast. The mothers are kissing and licking babies. All of these are very efficient ways of transferring microbes from one generation to the next.
That's the way it's always been for mammals, for the last 100 million years.
为了用另一种方式介绍这个主题,我提醒大家一下,我们人类是哺乳动物。
我们在无菌的子宫里开始我们的生命。
我们大量暴露于细菌和其他微生物是在羊水破裂时开始的,婴儿从产道中出生,身上包裹了母亲的微生物。
婴儿吞食这些微生物,而这时他们已经接触了母亲的皮肤和乳房,母亲们亲吻、舔舐婴儿。这些都是将微生物从一代传给下一代的非常有效的方法。
在过去的1亿年里,哺乳动物一直是这样传递微生物的。
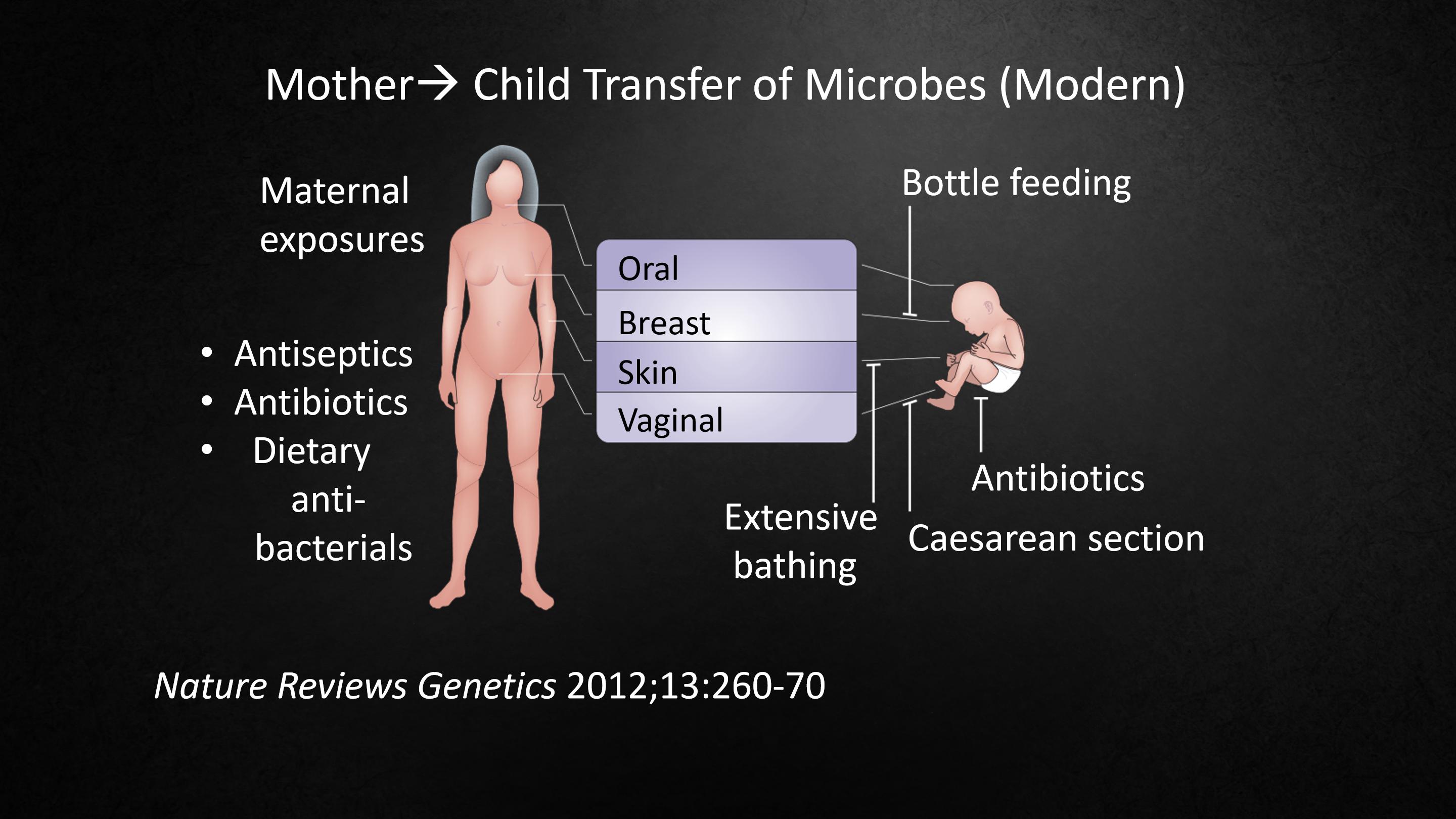
But these days, mothers are not the same as they used to be. They live in a world of antisepsis. They've taken many courses of antibiotics. They're eating foods that have antibacterials. And babies aren't the same either. They may be born by cesarean section.
Here in Shanghai, about one baby out of two is born by cesarean section. They're missing that first exposure to their mothers' microbes. They're bathed extensively. They're given formula which is only superficially like human milk.
And of course, babies are getting a lot of antibiotics.
但现在,母亲和以前不一样了。她们生活在一个抗菌的世界里,她们服用了很多抗生素,她们在吃含有抗菌药物的食物。而且婴儿也和以前不一样了,他们可能是通过剖腹产出生的。
在上海,大约两个婴儿中就有一个经由剖腹产出生,他们错过了第一次接触母亲微生物的机会,他们被冲洗得很干净,他们喝的是仅仅和母乳相似的配方奶粉。
当然,婴儿们会接触到大量的抗生素。
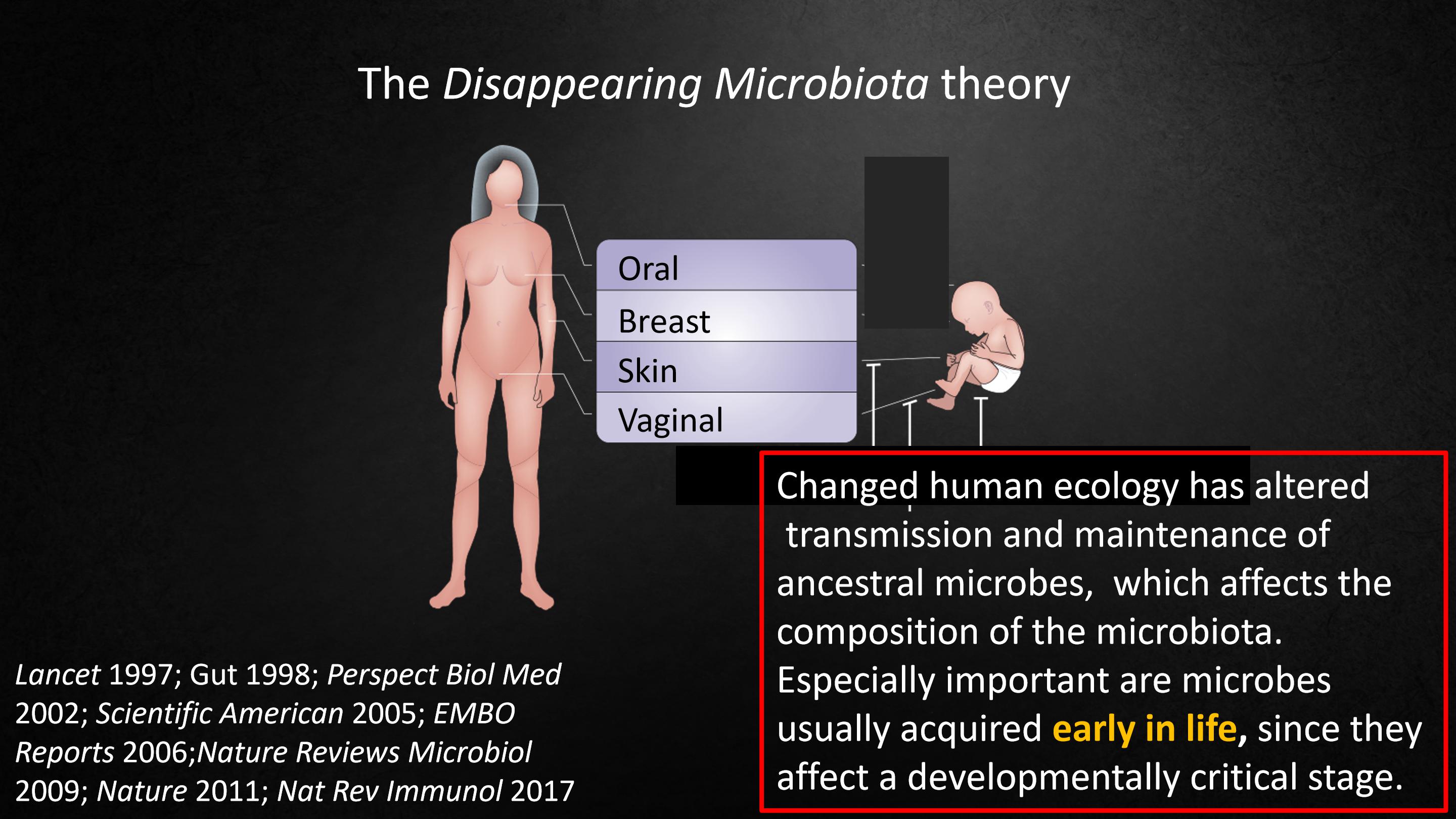
Because of this, over the last 20 years I've been thinking of an idea that I call the disappearing microbiota theory.
And it has two main ideas.
The first is that human ecology is changing, and it has altered the transmission of these microbes, and their maintenance of our very ancestral microbes.
And that affects the composition of what we're carrying. And especially important are the microbes that are usually acquired early in life, in childhood, since they affect a critical stage in development.
正因为如此,在过去的20年中,我一直在思考一种我称之为消失的微生物的理论。
它有两个主要的观点。
首先,人体生态正在发生变化,而且它已经改变了这些微生物的传播以及对我们祖先的微生物的保持。
这会影响我们携带的微生物的构成,尤其重要的是通常在生命早期和童年获得的那些微生物,因为它们影响发育的关键阶段。
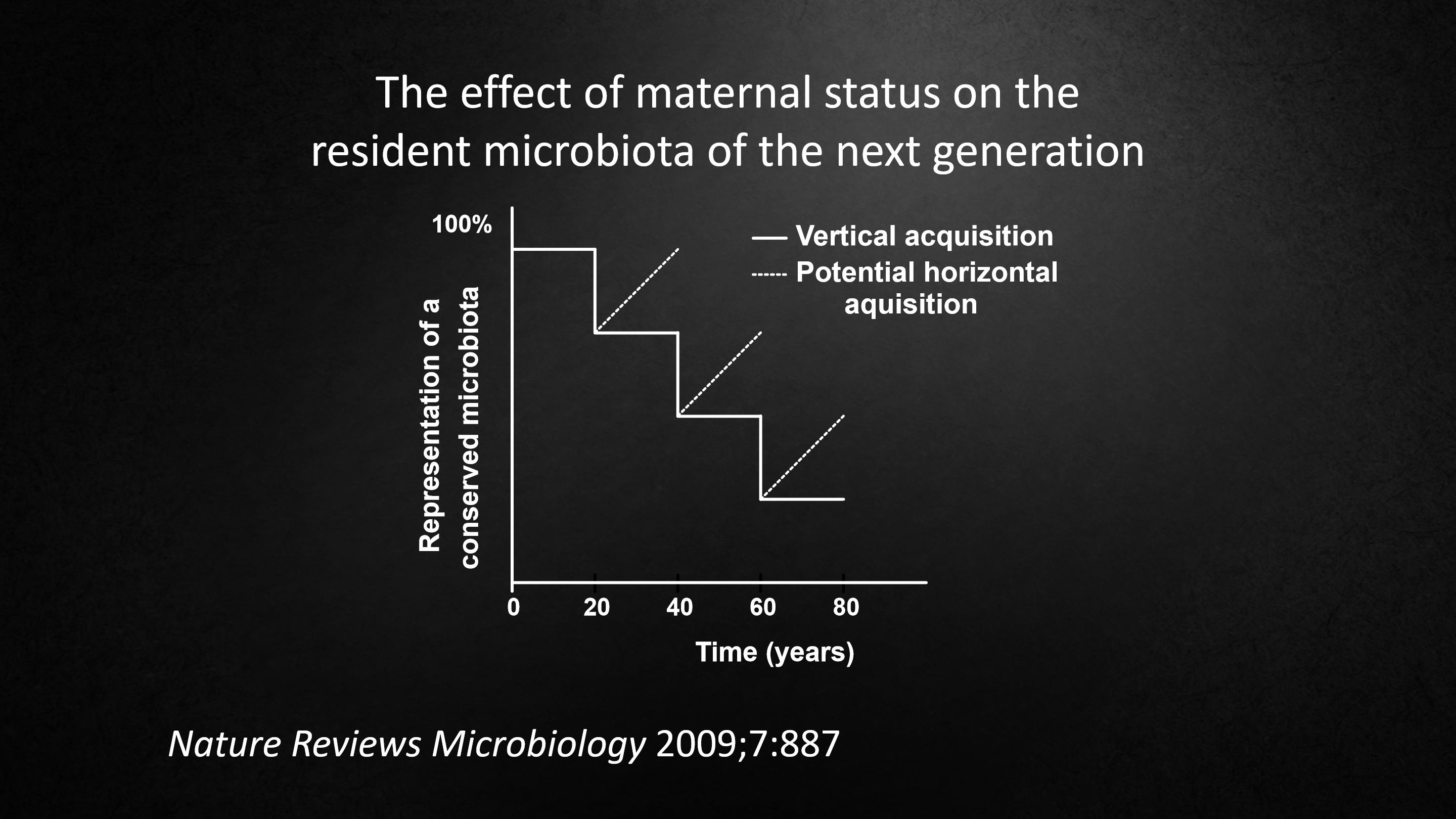
A few years ago, we extended this idea, and it's shown here, the effect of the mother's status of the microbiota of the next generation.
Our idea of ancient mothers is that they had ancient microbes.And if, before the next generation was born, they lost a few, maybe they could regain them horizontally.But if they lost them and they couldn't regain them, then the next generation would be born at a deficit. And so on, and so forth.
So that the change in each generation is cumulativeIt's not that it resets with each generation, but that it gets worse with each generation. This was our idea.
几年前,我们加强了这个想法,这里展示了母亲菌群的状态对下一代的影响。
我们认为,古代母亲拥有古老的微生物们。如果在下一代诞生之前,她们失去了一些微生物,也许可以水平地复得它们,但如果不能失而复得,下一代会在一个微生物不足的环境中出生,等等,等等。
每一代的变化都是累加的,并不是每一代会清零,而是每一代都变得更糟。这就是我们的想法。
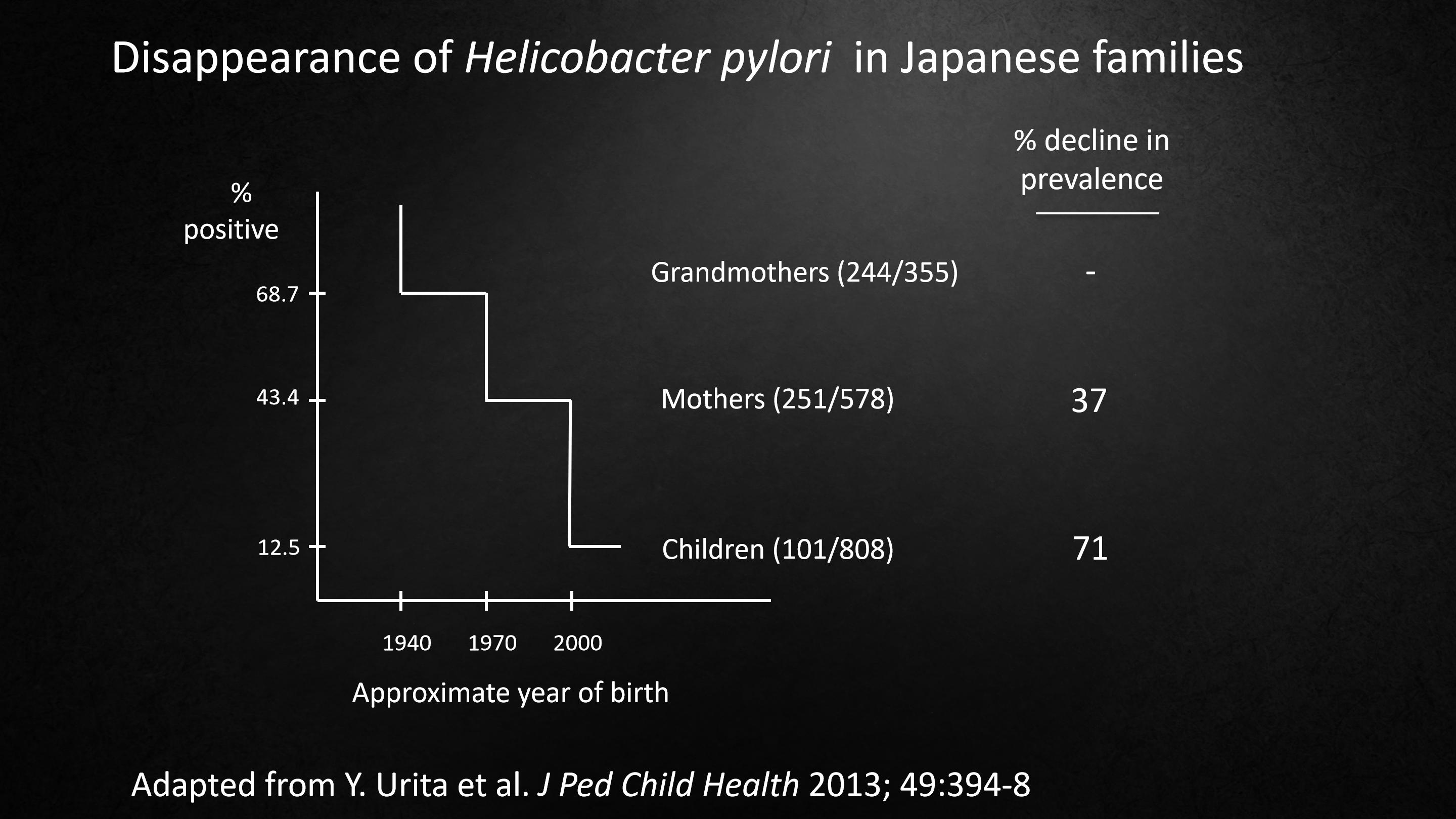
And fortunately, there's now evidence supporting this idea.
We talk about helicobacter pylori, which used to be the most common organism, the most important organism in the human stomach.
And here in this study of three generations in Japan, you can see the same kind of step down that we were worried about.
幸运的是,现在有证据支持这个观点。
我们讲到幽门螺杆菌,过去是最普通的生物体,也是在人类胃里面最重要的生物体。
这里是关于日本三代人的研究,大家可以看到我们所担心的同样退变。
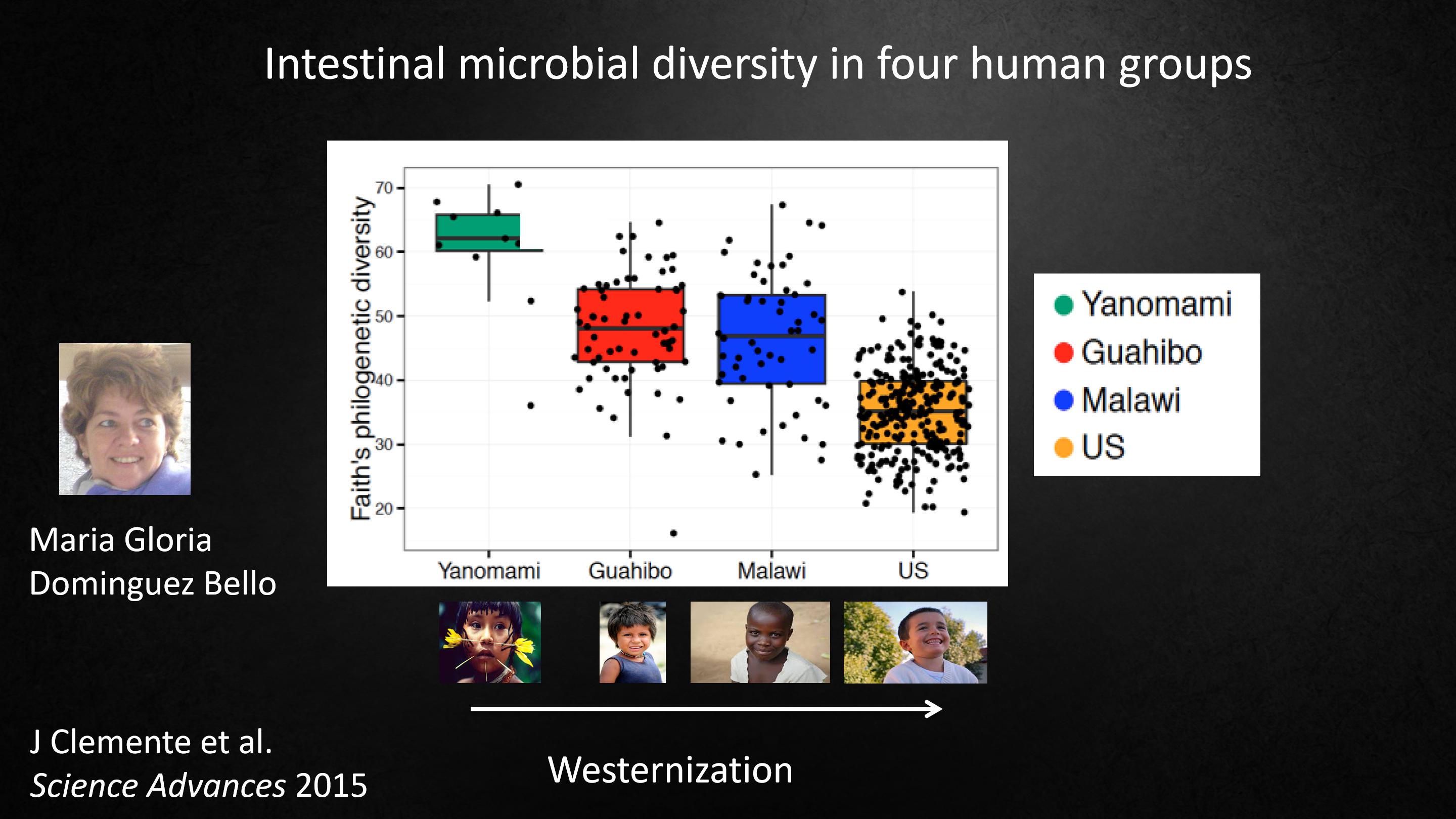
We can look at the overall diversity of microbes in the human body.
And this is work by Maria Gloria Dominguez, who's my wife, and she's right there.
Gloria looked at the total amount of diversity in the intestinal tract in children in the United States, and people in Africa and South America.
In a group of uncontacted Amerindians, they had never seen any kind of medical care.
And what she found is that the Amerindians had the greatest diversity. And we people in the United States, had the least. And you can almost imagine that step going down. And comparing the Amerindians to us, it suggests that we have already lost half of our diversity, that it's already gone.
我们可以看到人体内微生物的整体多样性。
这是我的妻子 Maria Gloria Dominguez 的成果,她今天也在场。
Gloria 调研了美国儿童,以及非洲、南美洲的人们肠道内的物种的总多样性。
在一组与世隔绝的印第安人中,他们从未接受过任何形式的医疗护理。她发现,印第安人的微生物组具有最大的多样性。
而我们美国人的多样性最少,你几乎可以想象到多样性的逐步下降。拿印第安人和我们比较,表明我们已经失去了一半的微生物多样性,它们已经消失了。

So what could be causing this?
I think there are many causes. But I'm going to highlight just one, and that's antibiotics.
All of us in this room know that antibiotics are one of the greatest discoveries of the 20th century.
There's a picture of Fleming, reenacting the discovery of penicillin. Antibiotics have saved countless lives. They've influenced every area of medicine.
那么这是什么原因造成的?
我想原因有很多。但我要强调其中一个,那就是抗生素。
在座的每一个人都知道,抗生素是二十世纪最伟大的发现之一。
这是一张 Fleming 的照片,重现了青霉素的发现。抗生素挽救了无数人的生命,它们影响了医学的各个领域。

And as a result, we've been using antibiotics more, and more, and more. How much more?
It's estimated that each year we're using more than 70 billion doses of antibiotics.
That's 10 doses of antibiotics for every man, woman and child on earth.
In the United States, we, on average, we have 833 courses per 1000 population. So that's five courses for every six people, year after year.
In children under two, they've had almost three courses of antibiotics. By the time they're 10, 10 courses of antibiotics. Pregnant women, just before the transfer of microbes, more than half of them are getting antibiotics.
结果我们越来越多的使用抗生素,有多频繁?
据估计,我们每年都要使用700亿剂以上的抗生素,也就是地球上每个男人、女人和孩子使用10剂抗生素。
在美国, 我们每1000人平均使用833疗程的抗生素治疗,也就是每6个人接受5个疗程,年复一年。
在2岁以下的儿童中,他们已经接受了将近3个疗程的抗生素治疗。等他们长到10岁,就有10个疗程。就在微生物传递之前,超过半数的孕妇正在使用抗生素。
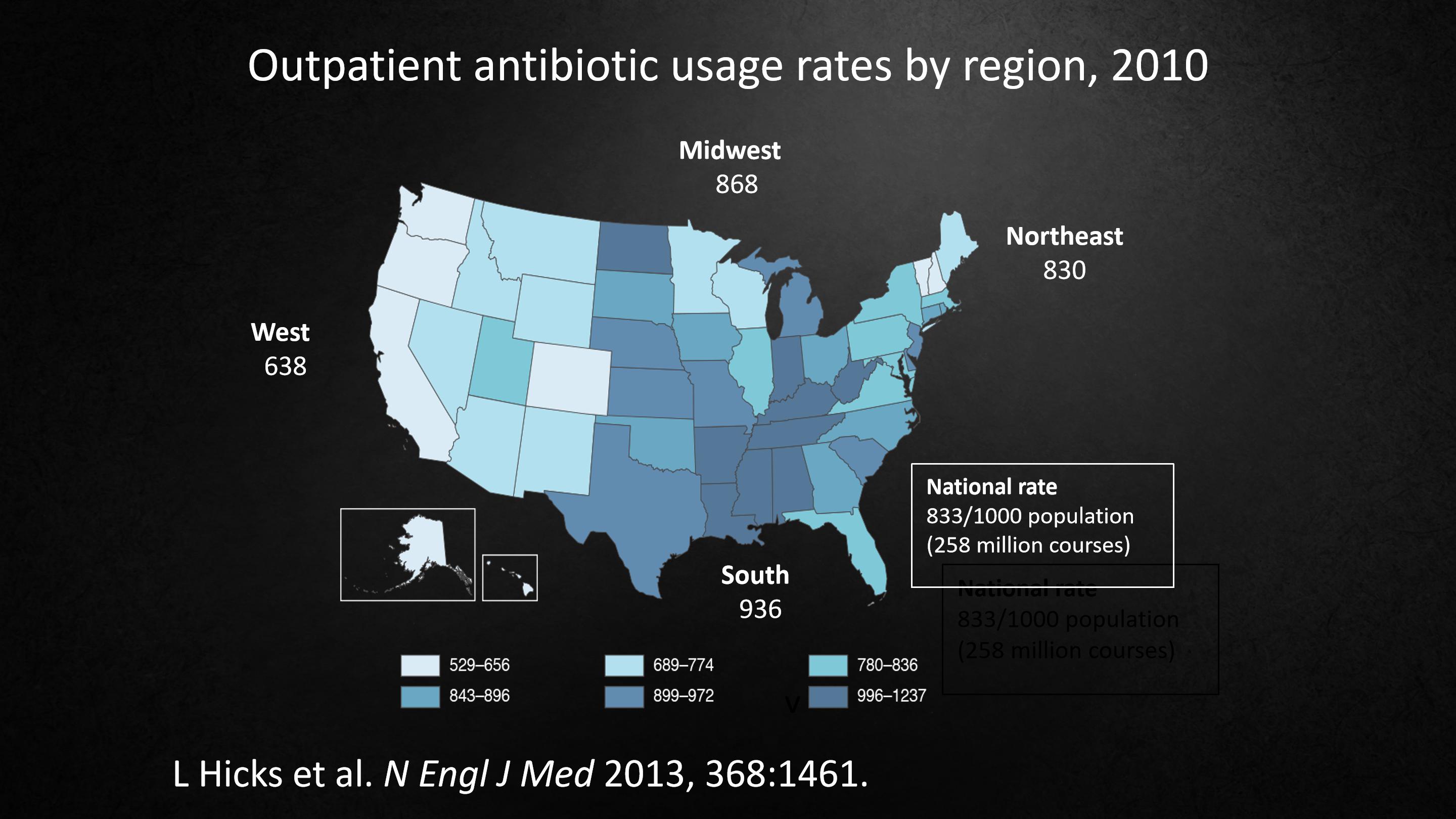
Antibiotic use varies tremendously Doctors. Some doctors prescribe it a lot, some hardly prescribe it.
If we look at the map of the United States, the national average is 833 per 1000.
In the northeast and the Midwest, it's similar to the average. But in the west, it's much less. In the south it's much more. Between the west and the south, there's a 50% difference, but there's no 50% difference in the rate of serious bacterial infection.
This reflects differences in culture, in practice, not medical necessity.
抗生素使用也有巨大差别,一些医生在处方中开很多抗生素,一些医生几乎不开。
如果我们看着美国的地图,全国平均1000人使用833疗程抗生素。
在东北部和中西部,与平均值相当;但在西部,要少很多;南部又要多出平均值很多。在西部和南部之间,有50%的差异,但严重细菌感染率没有50%的差别,这反映了文化、实践并不是医疗必要性的差异。
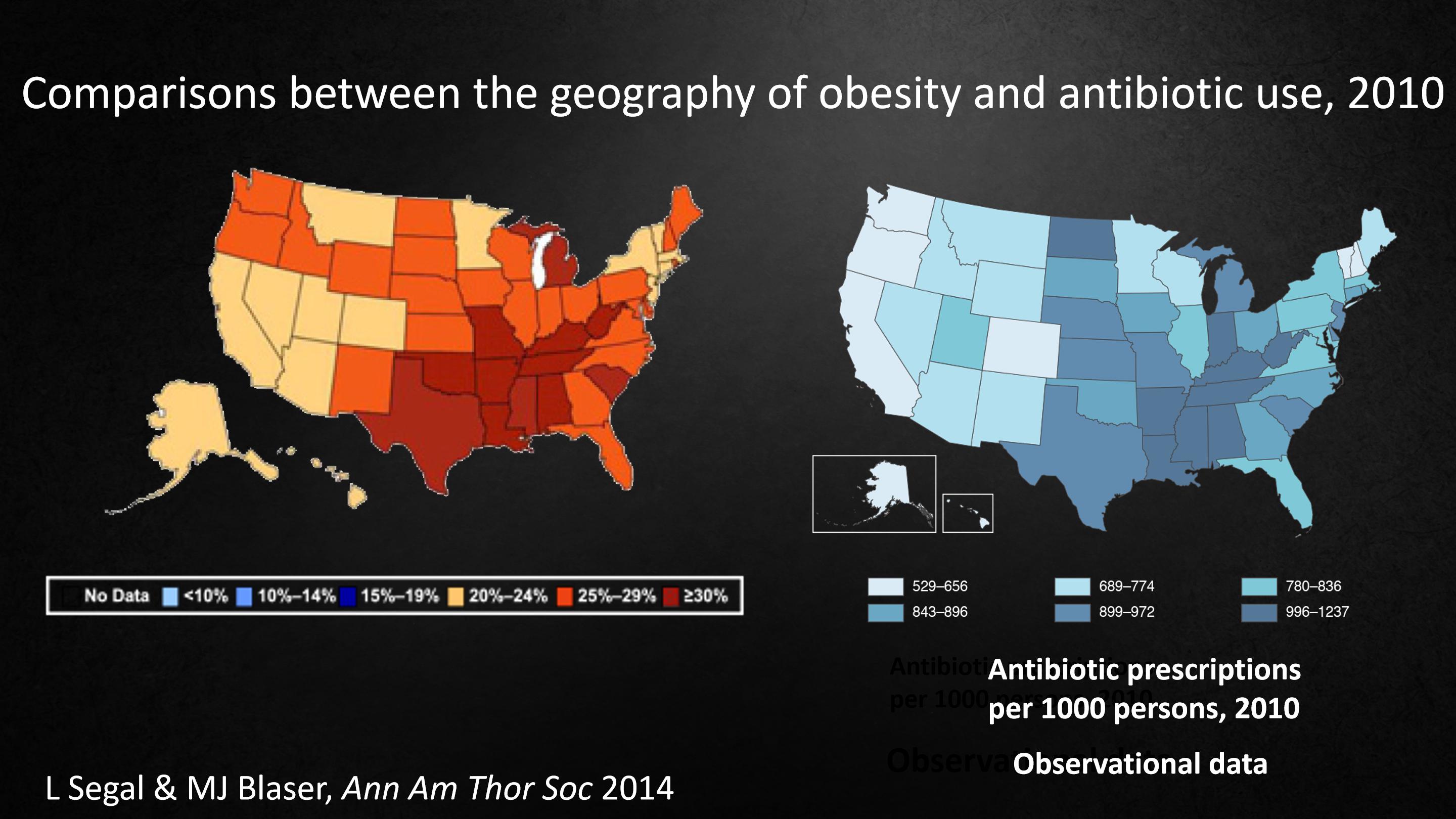
So I think it's interesting to compare these two maps from the Center for Disease Control in 2010. On the left, obesity. On the right, antibiotic use.
And if you look at the maps, they look very similar. It's not random.
But these are observational data. They don't tell us anything about cause. Could antibiotics cause obesity? Could obesity cause people to use antibiotics? But they get our attention.
我认为比较这两张2010年的地图很有意思,它们来自于美国疾病控制中心。
左边,肥胖。右边,抗生素。
如果你看地图,会发现它们看上去很相似。这不是偶然。
但这些都是观测数据,它们没有告诉我们任何原因,抗生素能引起肥胖吗?肥胖会导致人们使用抗生素吗?但它们引起了我们的注意。
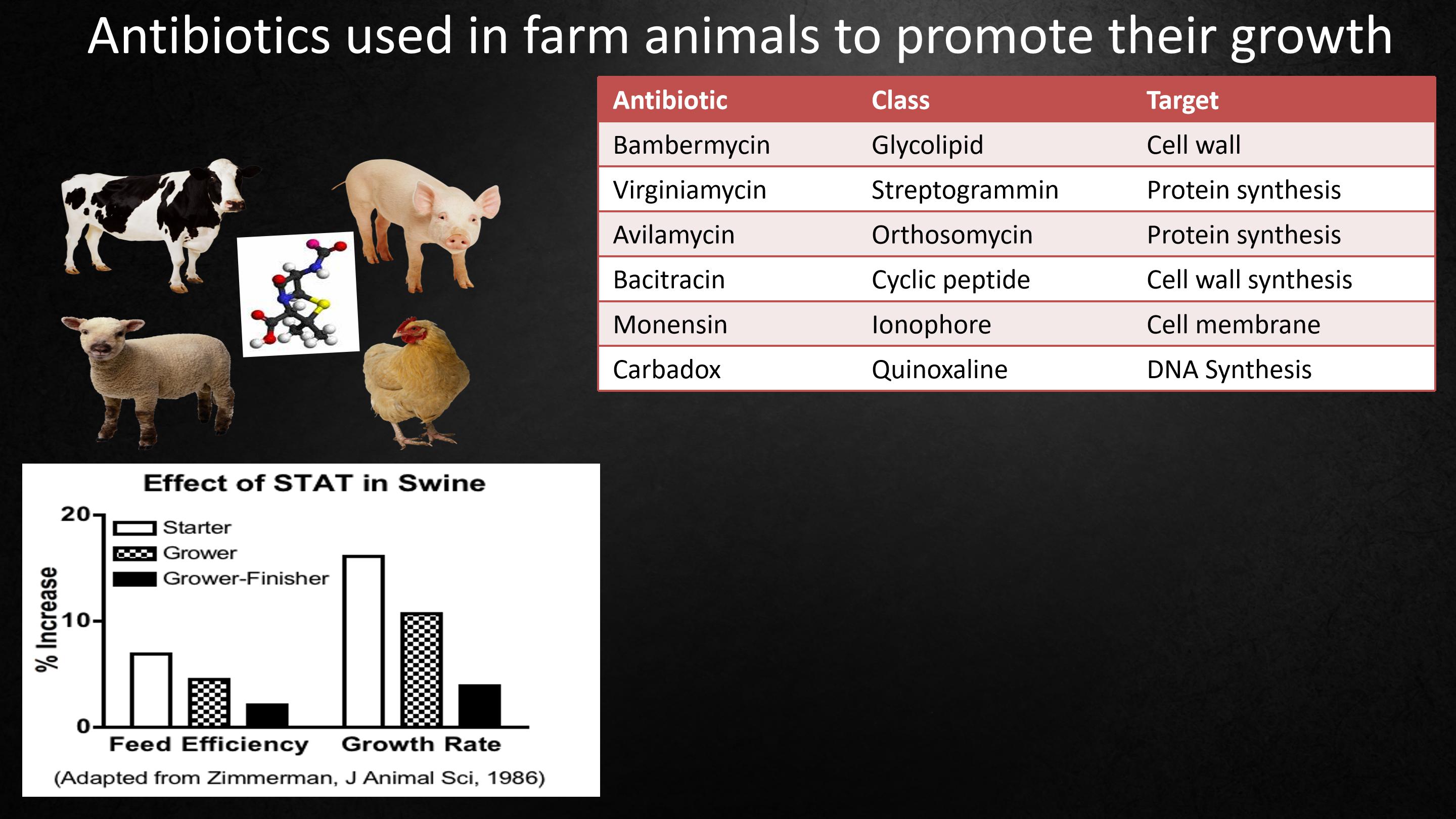
But in fact, we've known for 70 years that antibiotics affect metabolism.
Because farmers use antibiotics to improve the growth of their livestock. Antibiotics work between chickens and cows, a very wide swath of vertebrate evolution. Antibiotics work as antibacterials, regardless of their chemical structure, their class, their target, their spectrum. Antivirals do not work.Antifungals don't work.
Very importantly, the farmers found that the earlier in life they start the antibiotics, the bigger the effect. And this suggested to us that antibiotics are affecting development.
实际上,关于抗生素会影响代谢,我们已经知道了70年。
因为农民使用抗生素来促进牲畜的生长,抗生素对鸡和牛都起作用,它们是脊椎动物进化进程中非常广泛的分支。抗生素被当作抗菌药物,不管它们的化学结构、种类、目标、范围如何。抗病毒药物不起作用,抗体也失去作用。
非常重要的是,农民们发现越早开始使用抗生素,影响就越大,这也向我们暗示抗生素正影响发展。
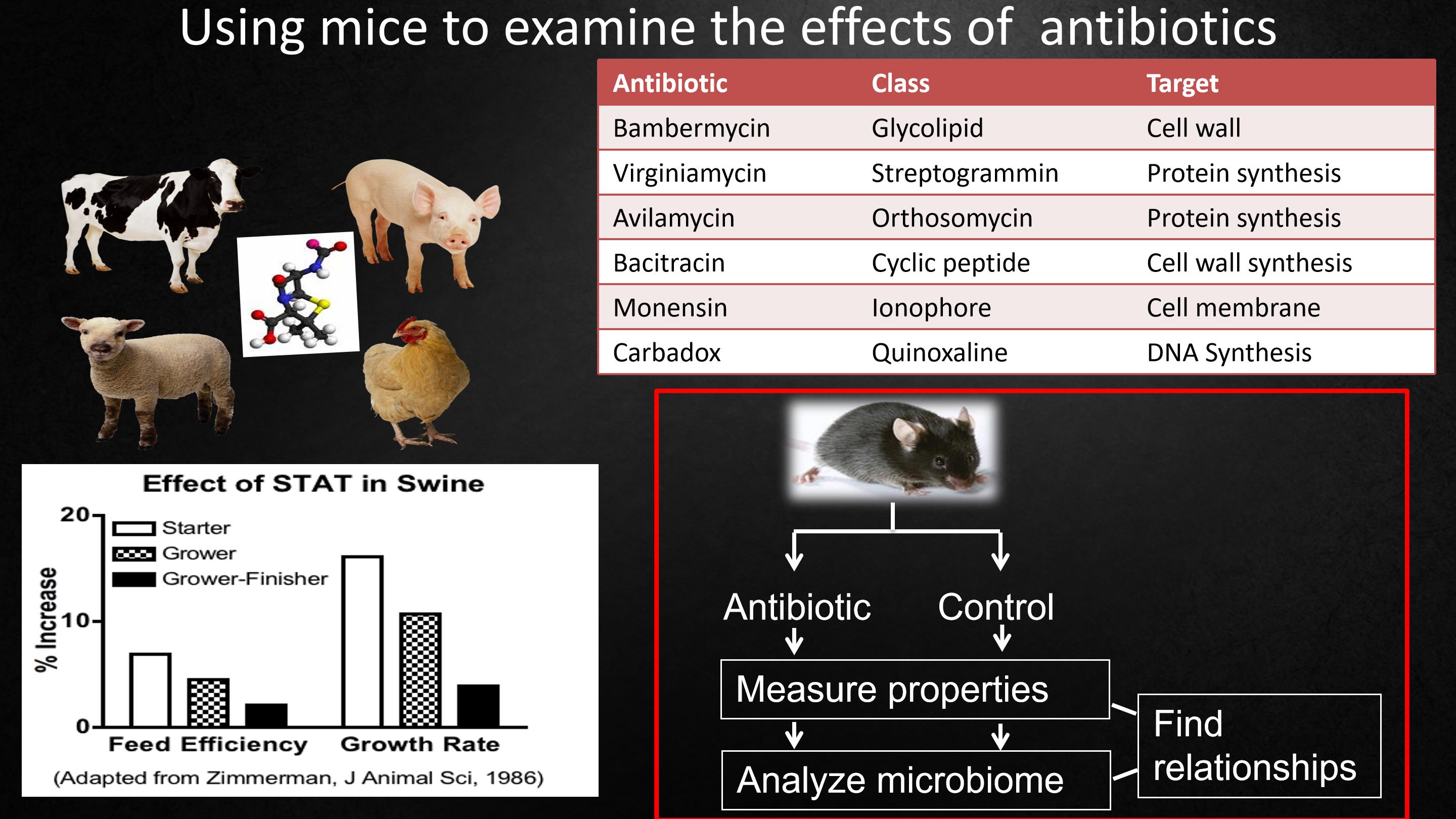
So we began to do studies in mice, where we could study it very carefully. Where we would give mice antibiotics or not. Asked what happened to the mice? What happened to their microbiome? And see if we could find relationship.
于是我们开始在小鼠身上做研究,这样我们可以非常仔细地研究它。我们给小鼠使用抗生素,探究小鼠身上发生了什么?它们的微生物组发生了什么?看看我们是否能找到关联。
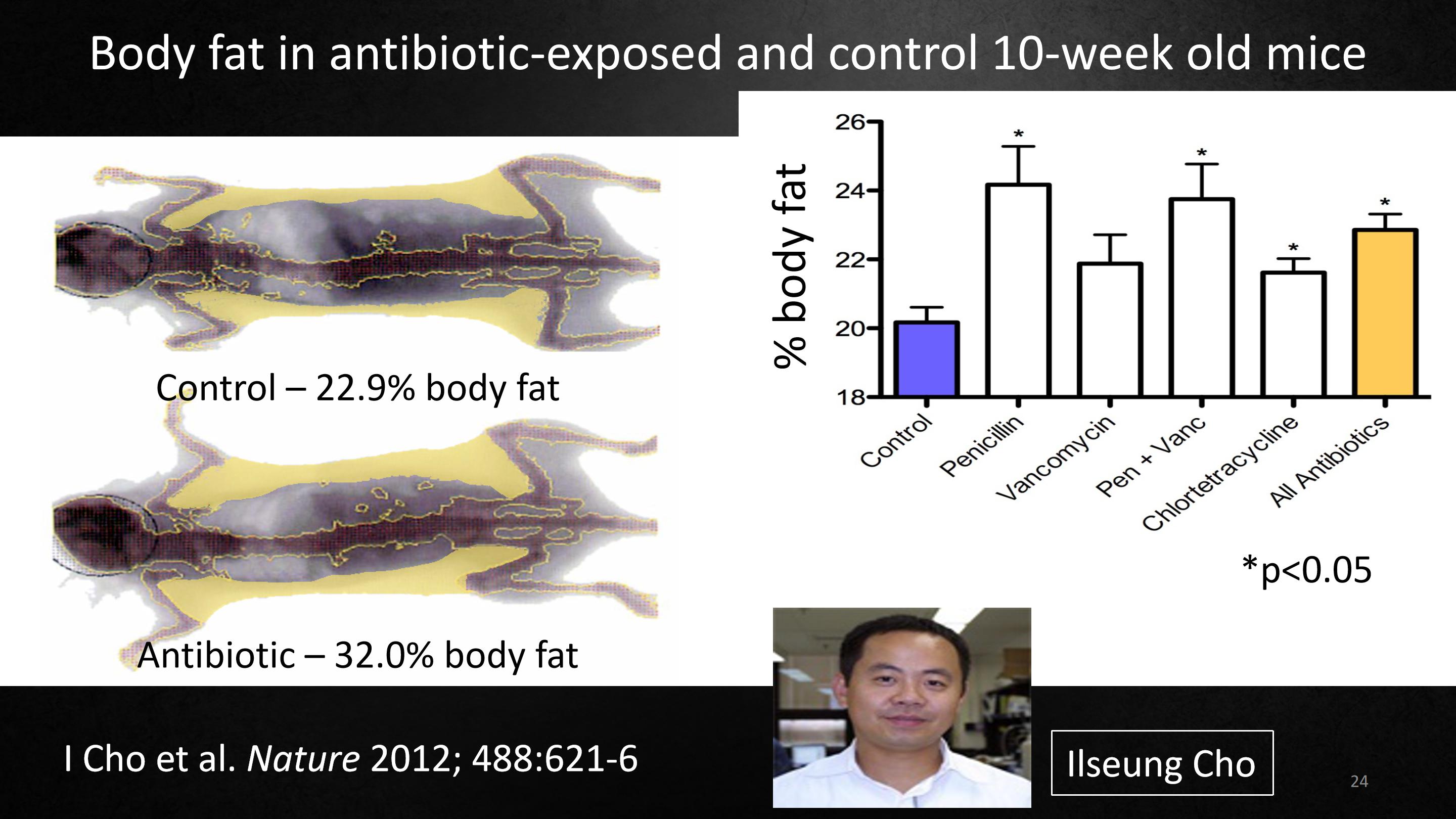
I'm going to show you a few of our results. Our first studies were done by Dr. Ilseung Cho when he worked in my lab. He wanted to know what's the effect of antibiotics on body fat.So he gave mice four different antibiotic regimens at the midpoint of the level approved for use on the farm.
And in this graph, you can see that the mice that got antibiotics had more body fat than the control mice that did not get antibiotics. This was our first evidence that antibiotics were changing metabolism in the mice model. And you can see it in these pictures of the mice as well.
我要给大家展示一些我们的成果。
我们第一个研究是 Ilseung Cho 博士在我实验室工作期间完成的,他想知道抗生素对体脂有什么影响。他使用了批准用于养殖场的中间剂量,给小鼠制定了四种不同的抗生素方案。
在这张照片中,接受抗生素的小鼠比未接受抗生素的对照小鼠拥有更多的体脂。这是我们的第一个证据证明抗生素会改变小鼠模型的新陈代谢。大家也可以在这些小鼠的照片上看出来。
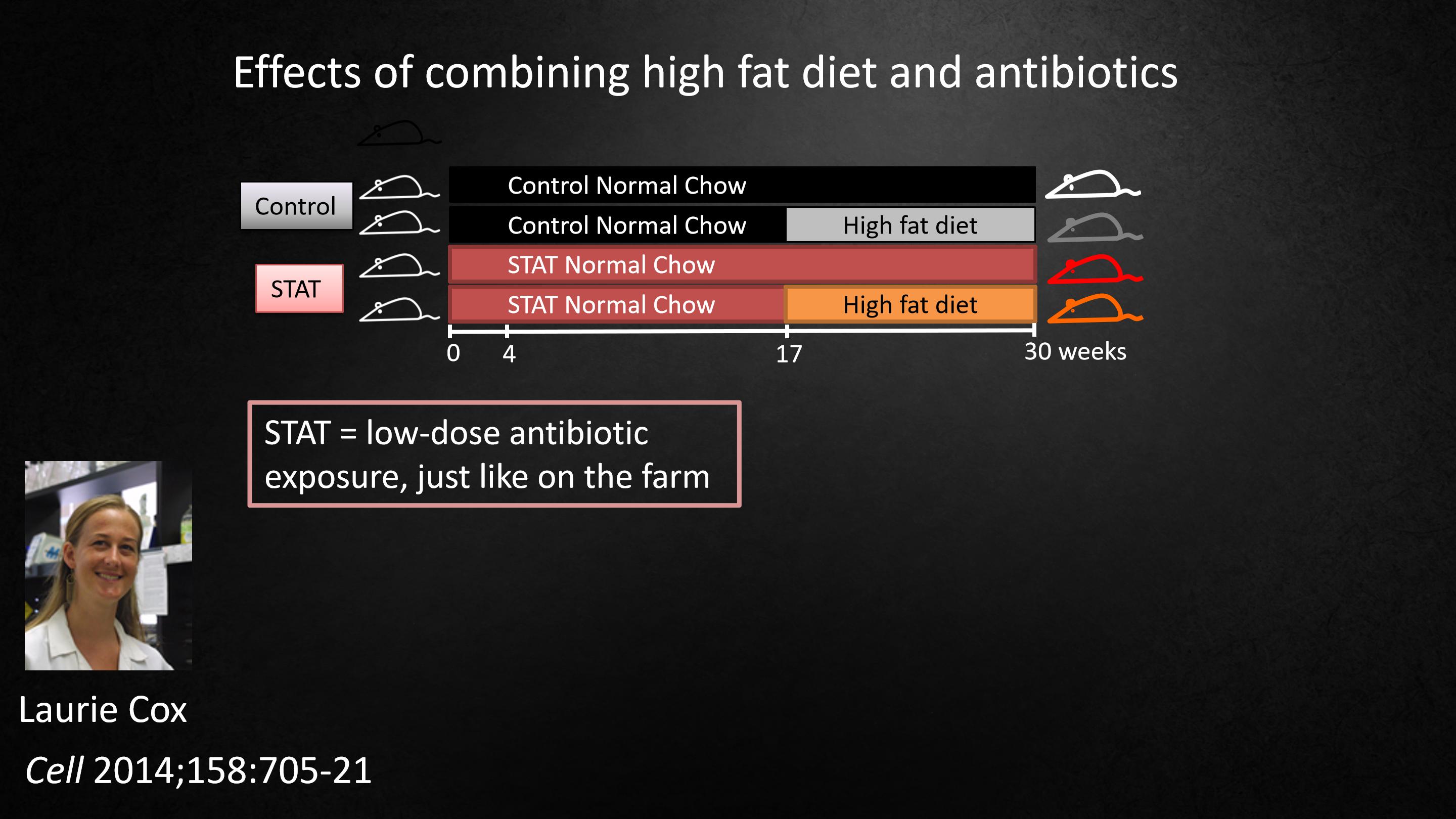
So this work was continued by Laurie Cox when she was a graduate student in my lab.
She asked what happens if she combined a diet that's high in fat, high in calories, with antibiotics. Would there be additive effects? So she gave mice penicillin, or not.And then, at week 17, half the mice were put on a high-fat diet. She used the same kind of antibiotic regimen that farmers use.
这项工作后来由我实验室的研究生 Laurie Cox 继续推进。
她想探究如果把高脂肪、高热量的饮食和抗生素结合在一起会发生什么。会有叠加效应吗?于是她给一些小鼠注射青霉素,另一些不注射,并喂它们吃正常的食物。接着,在第17周,其中一半的小鼠吃高脂食物。她使用的是与农民们使用的一样的抗生素。
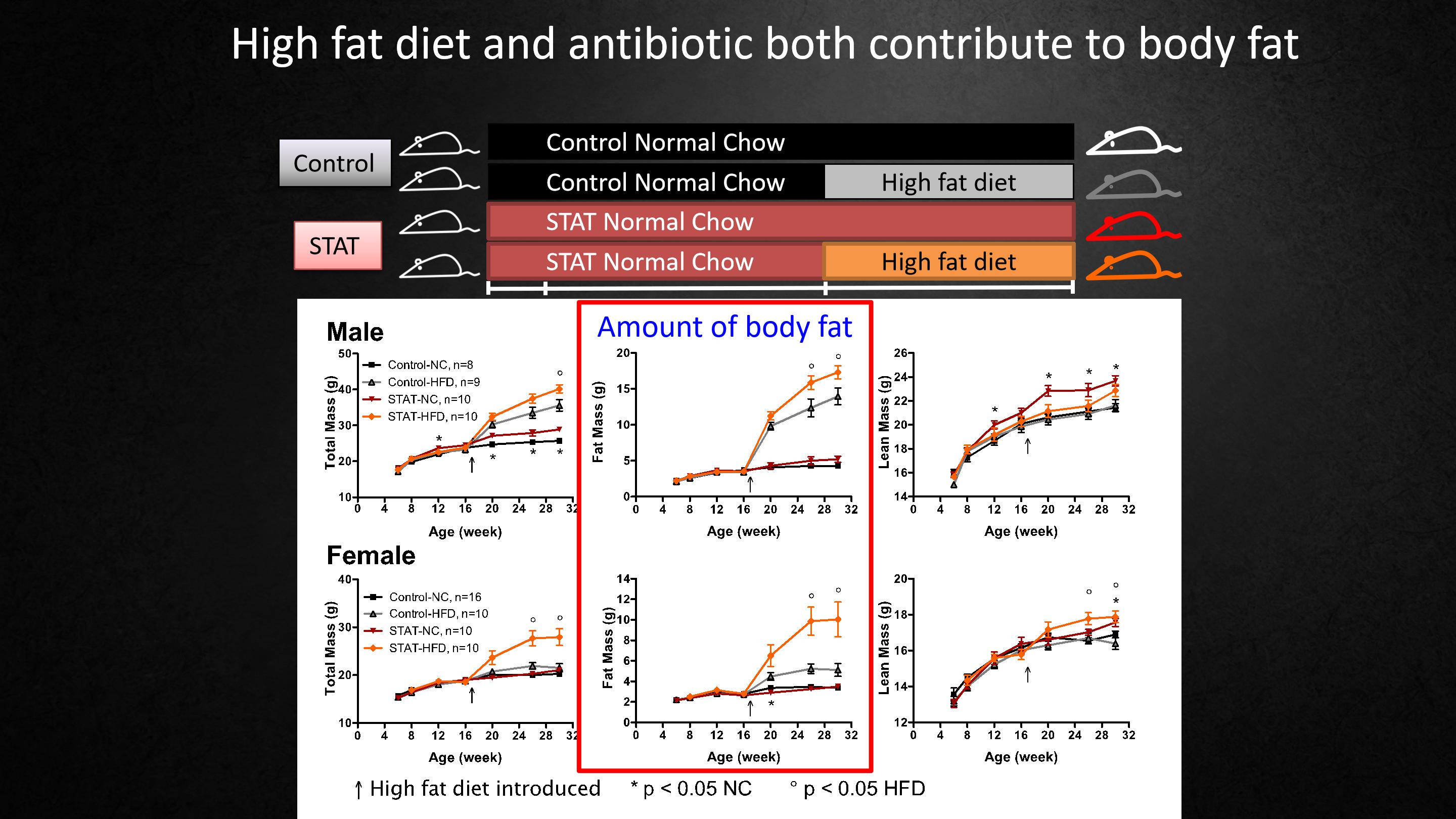
So in the mice that were put on a high-fat diet, that's the black line.
They gained a lot of fat. But if they were on high-fat plus antibiotics, they gained even more. That was male mice on the top, and female mice it's similar, but it's worse.
The female mice on the high-fat diet gained five grams of body fat. High-fat diet plus penicillin, 10 grams.It doubled the amount of body fat. So the antibiotic potentiated the effect of the high-fat diet. Up to this point, the mice were getting antibiotics for their whole life.
她得到很多结果,我想把重点放在身体脂肪上,显示在图片的中间。
在高脂饮食的小鼠身上,由黑线显示的它们长了很多脂肪。但如果它们在高脂饮食再加上抗生素的状况下,它们会长更多脂肪。在顶部的是雄性小鼠,雌性小鼠也类似,但更严重。
高脂饮食的雌性小鼠体重长了5克,高脂饮食加上青霉素,长了10克。它使体内脂肪的量增加了一倍,所以抗生素增强了高脂饮食的效果。到此刻为止,小鼠在一生中都在使用抗生素。
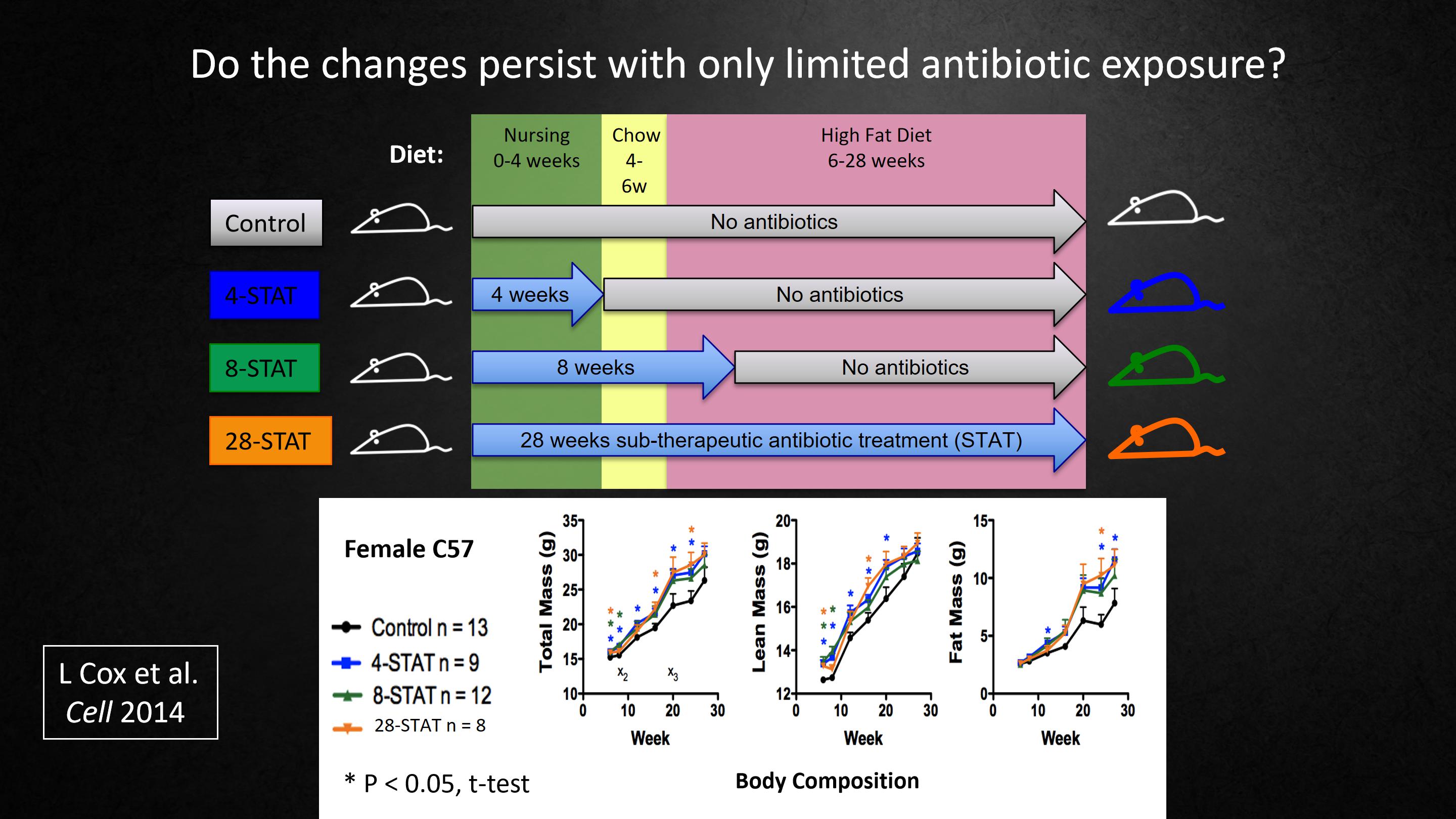
So next we asked, would the changes persist if the antibiotic exposure was much shorter?
So in addition to lifetime antibiotics, we only gave antibiotics for 8 weeks, or only for 4 weeks. Here's the effects on total mass, muscle mass, fat mass. All the antibiotic regiments had the same effect. So even 4 weeks was enough. That was enough for the full effect.
接下来我们会问,如果接触抗生素的时间变短,这些变化还会持续吗?
在终生使用抗生素之外,我们在一些小鼠身上,只给了8周抗生素,或只有4周。这是对总质量、肌肉量、脂肪量的影响,所有的抗生素组合都有同样的效果。所以只要4周就足够了,这就足够造成完全的影响。
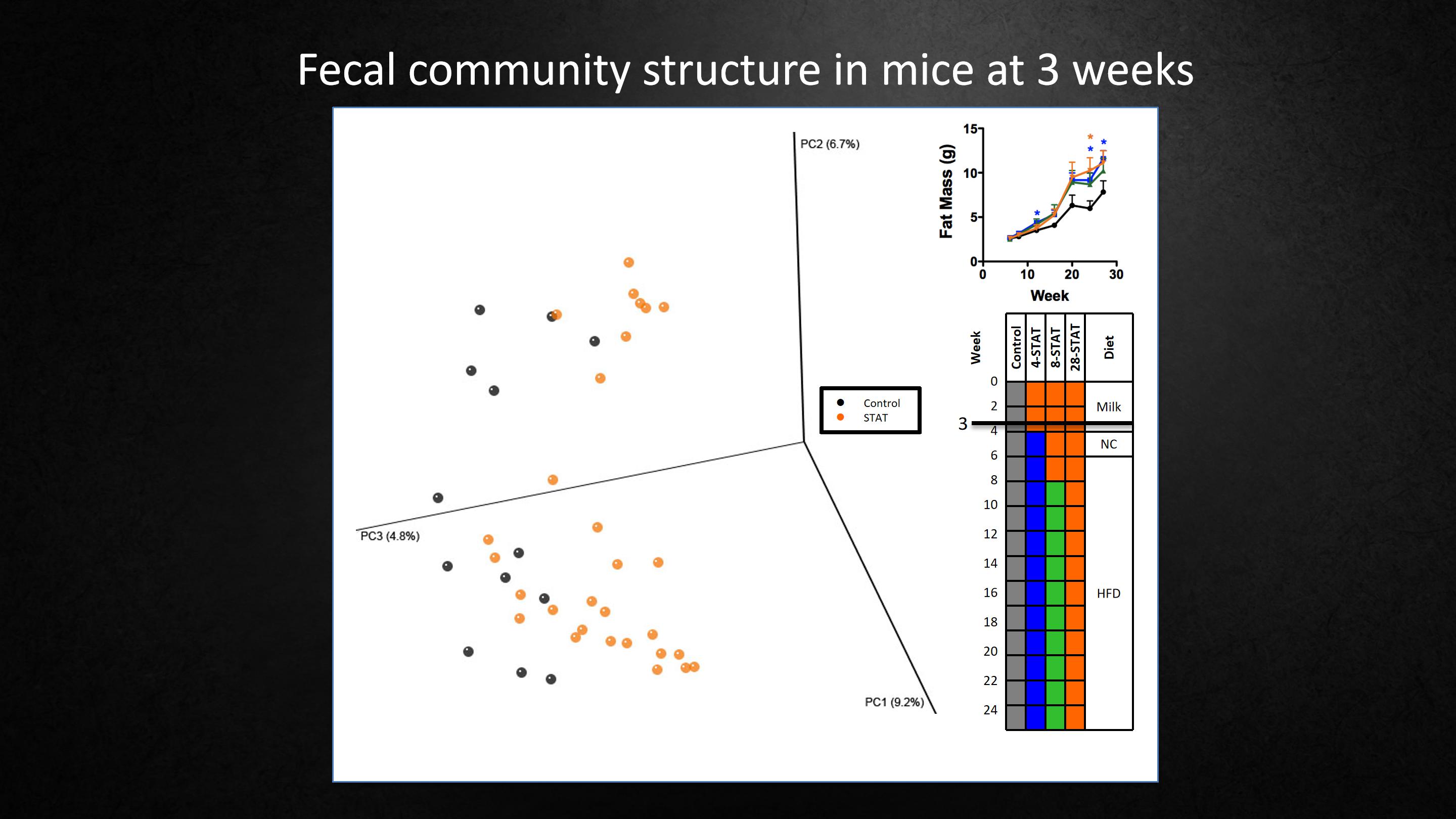
So then we were interested to see what's the effect of the antibiotic on the microbiome. So this slide is a little complicated. I'm going to tell you about it very slowly.
First, we're going to look at what is the composition of the microbiome in the mice that are 3 weeks old. And at 3 weeks, really there are only two groups of mice. The mice that received antibiotics shown in orange, and the mice that didn't receive, the control, shown in black. On the left side is what we call a principal coordinates analysis. Each dot is the composite of the microbiome in one mouse.
And what we can see is that the black dots and the orange dots are similar in their distribution, but they're not identical.That's not surprising. One group is getting antibiotics, the other is not.
接下来我们很有兴趣想看到抗生素对微生物的影响是什么?这张幻灯片有点复杂,我会很慢地向大家讲解。
首先,我们要去看看3周大的小鼠的肠道菌群是由什么组成的。在3周的时间里,只有两组小鼠,接受抗生素的小鼠用橙色表示,而那些没有接受抗生素的对照组小鼠则用黑色表示。在左边是我们所说的主坐标分析,每一个点代表一只小鼠的微生物组成。
我们能看到的是黑点和橙点在分布上相似,但又不完全相同,这并不奇怪。其中一组持续使用抗生素,另一组没有。
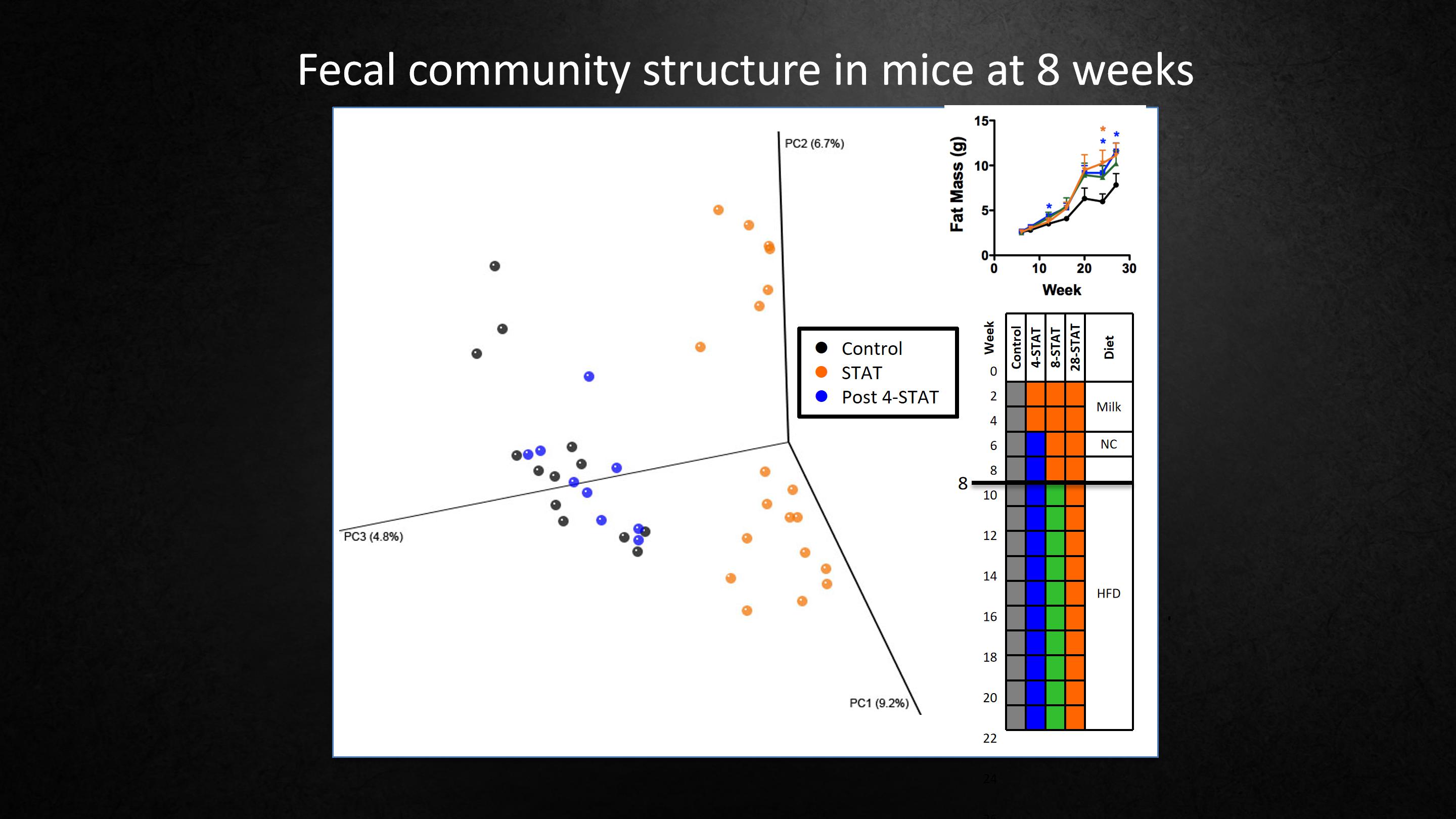
Now we're going to look at 8 weeks. And at 8 weeks, we actually have three groups of mice.
Control mice, no antibiotics.Continued antibiotics,But we have another group in blue that got antibiotics for 4 weeks and then stopped. So now, when we look at the dots on the graph, we see, between the controls in black and the antibiotics in orange, there's more distance. That's not surprising.
One group is getting antibiotics. But the group that got antibiotics then stopped, their microbiota have become normal. But the effect on the body fat is permanent. So this was our most important evidence that if we change the microbiota early in life, even if it's short, it will have permanent effects.
现在我们看看使用抗生素8周的小鼠,实际上我们有三组小鼠使用了8周的抗生素。
对照没有使用抗生素的和持续使用抗生素的小鼠。另外我们有一组小鼠使用了4周抗生素后停药了,用蓝色表示。现在,当我们看图表上的点时,我们会发现以黑色标示的对照组和以橙色标示的抗生素组之间距离更大了。这并不奇怪。
其中一组持续使用抗生素。但是那组使用抗生素后又停药的小鼠,它们的菌群已趋于正常,但对身体脂肪的影响是永久性的。这是我们最重要的一个证据,证明如果我们在生命早期改变菌群,即使时间很短,也会产生永久的影响。
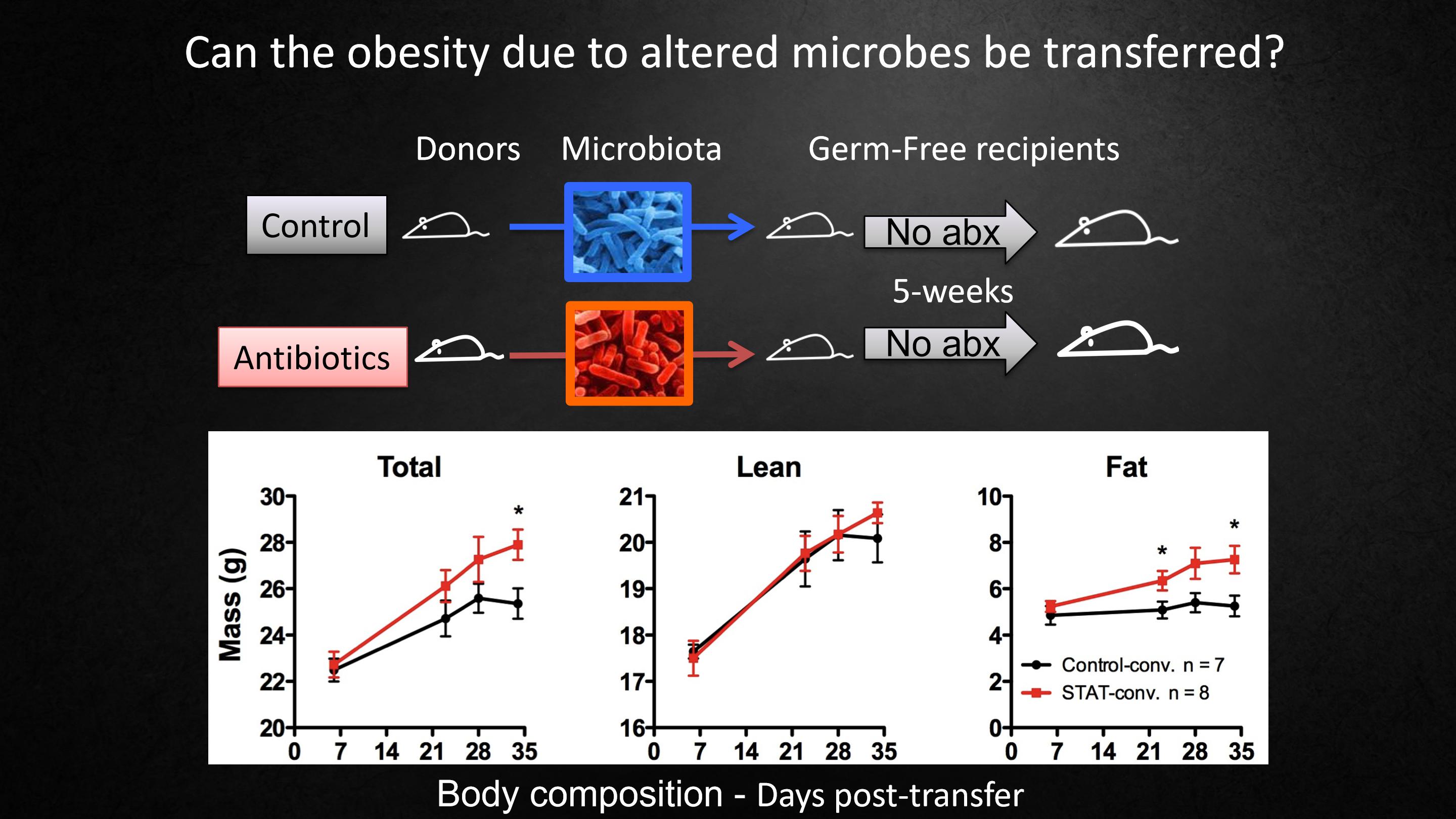
And we think that's what's happening in people as well.To understand this further, we did a transplant of microbes in mice that received antibiotics or did not. We harvested their microbes from their intestine, and we gave them to germ-free mice.
And now we're establishing their new populations. These are mice that had no bacteria at all.
And we followed these mice for the next 5 weeks.They did not receive any antibiotics. And at the bottom, we can see the effects. The black line is the control group. The antibiotic perturbed microbiota increased the total mass of the mice. It didn't affect their muscle mass, but it affected their fat mass. So the signal was in the microbiota, the altered microbiota is carrying the metabolic signal.
我们认为这样的事情同样会发生在人类身上,为了进一步了解,我们对有或没有使用抗生素的小鼠进行微生物移植,从它们的肠道里获取微生物,并把它们移植给无菌小鼠。
这些是完全没有细菌的小鼠,现在我们正在建立它们的新种群。
在接下来的5个星期里,我们跟踪这些小鼠的状况:它们没有接触任何抗生素。在底部,我们能看到这些影响。黑线表示对照组,受抗生素干扰的菌群增加了小鼠的总质量。它没有影响肌肉质量,但影响了脂肪质量,线索就在菌群中,被改变的菌群携带着新陈代谢指令。
Now, we've been interested in other diseases. Another student in the lab, Alexandra Livanos, was interested in type-1 diabetes.
Her idea was that early-life antibiotics would change the gut microbiome and lead to type-1 diabetes in a special kind of mouse that gets this spontaneously.
She hypothesized it would be due to changes in the expression of genes in the intestine, and to populations of t-cells in the intestine.
She's shown every part of this.She graduated and got her degree.
现在,我们对其他疾病产生了兴趣。实验室里的另一个学生,Alexandra Livanos,她对1型糖尿病感兴趣。
她的想法是,在一种特殊的小鼠中,在生命早期接触抗生素会改变肠道微生物组,并自发地导致1型糖尿病。
她推测这归因于肠道中基因表达和T细胞种群的改变。
她展示了其中的每一部分。她毕业并拿到了学位。
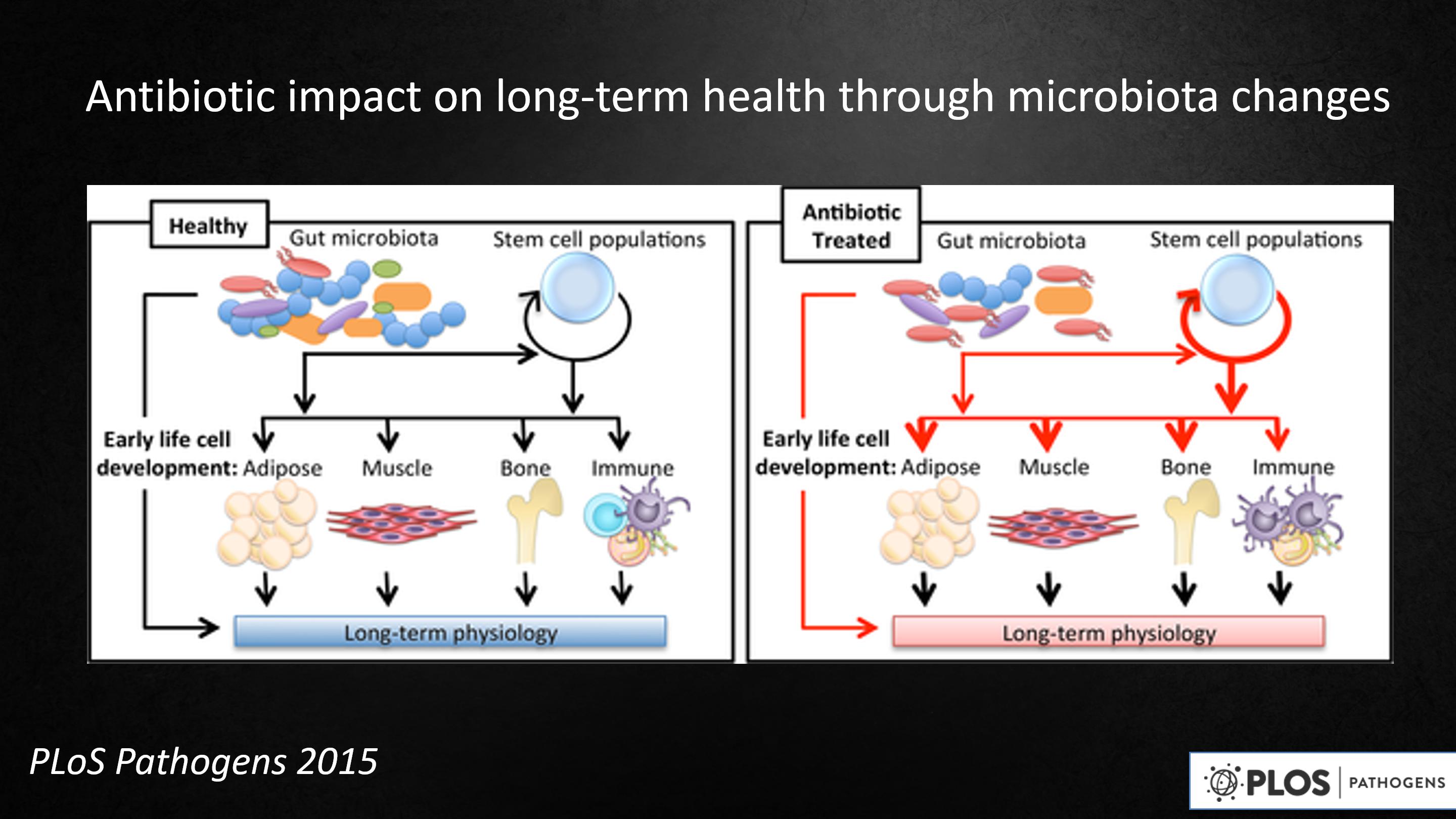
So let me begin to finish up by saying, our ideas that antibiotics are having an impact on long-term health by how they affect the microbiota.
Our idea is that, in health, the ancient gut microbes are talking to our stem cells, they're guiding them. Those conversations are telling them how much fat to develop, how much muscle, how much bone, what should their immune cells be like.
That early development leads to long-term development. But in antibiotic-treated individuals, or individuals who have missing microbes, the gut microbiota is different. The conversations are different.
The early-life development is different, and the long-term physiology is different. This is our major theory.
我开始作一些总结发言,我们认为抗生素通过影响菌群对健康产生长期的影响。
我们的想法是,在健康个体中,古老的肠道微生物能与我们的干细胞交流对话,前者引导着后者。这些对话告诉身体要长多少脂肪、肌肉、骨骼,以及免疫细胞要长成什么样。
早期的发育会影响长期发育,但在经过抗生素治疗,或在有微生物消失的个体中,肠道菌群是不同的,这些对话也是不同的。
生命早期的发育不同,长期的生理也不同,这是我们的主要理论。
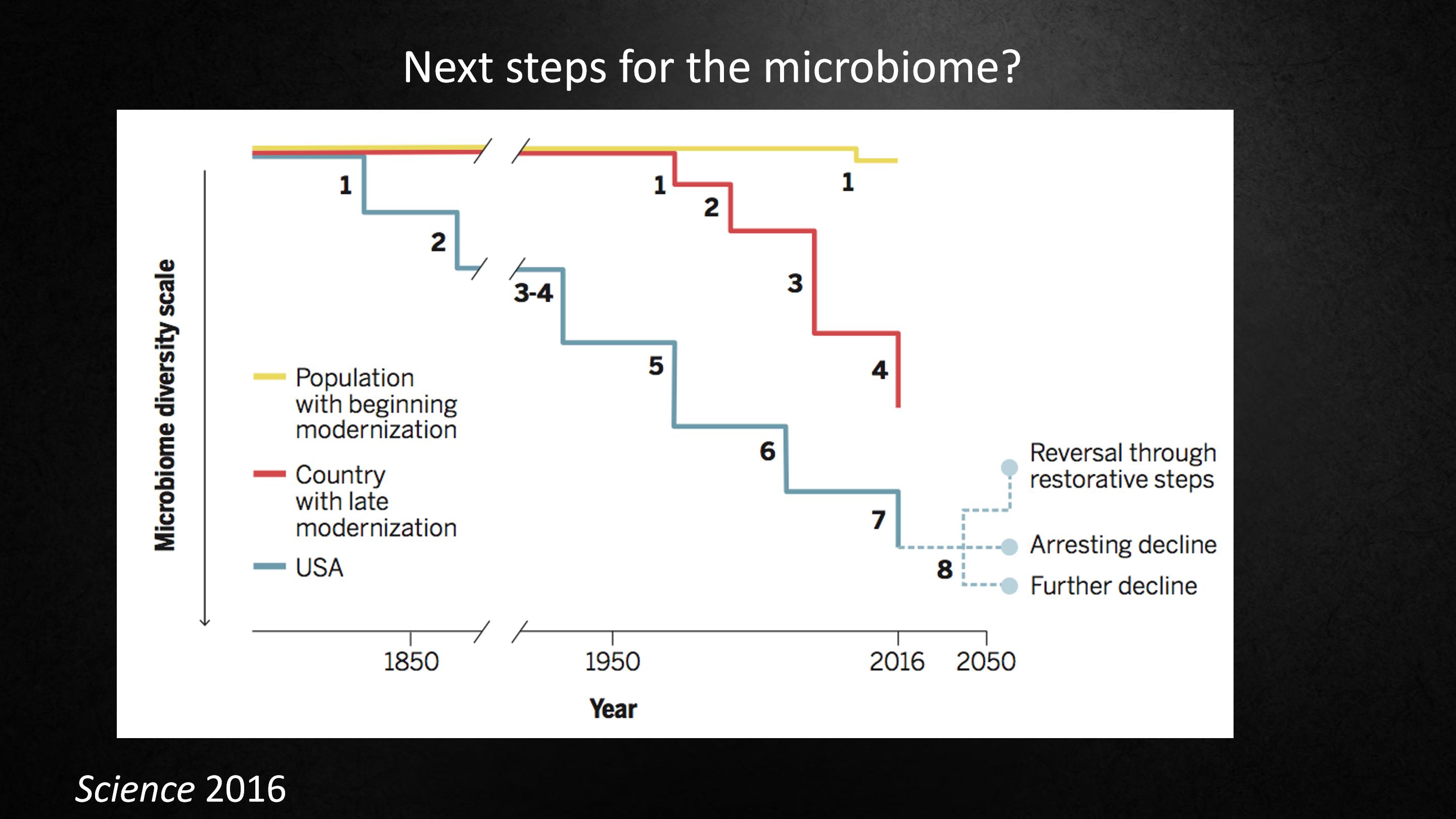
So what's the future going to bring?
Here, we go back to this idea of the step going down, each generation getting worse.
The blue line might be a country like the United States. The red line might be China. It started to develop later, but it's developing so rapidly. Maybe the yellow line is a country in Africa or Latin America that's just beginning to develop. So we're all going down.
What will the future bring?Will it continue to go down? Will we stop it from going down any further? Or will we begin to restore?
I think that we will have to begin to restore, otherwise we will have many of these modern plagues.
那么这会对未来带来什么呢?
这里,我们回到退变这个想法,每一代人会变得更糟。
蓝线代表的可能是一个像美国这样的国家,红线可能是中国,它开始发展得迟,但发展得却很快。也许黄线是一个在非洲或拉丁美洲的国家,才刚刚开始发展。在菌群多样性方面我们都在往下走。
未来会带来什么?还会继续走下坡路吗?我们能阻止它进一步往下走吗?还是我们会开始重构菌群多样性?
我认为我们必须开始重构,否则会出现许多现代瘟疫。
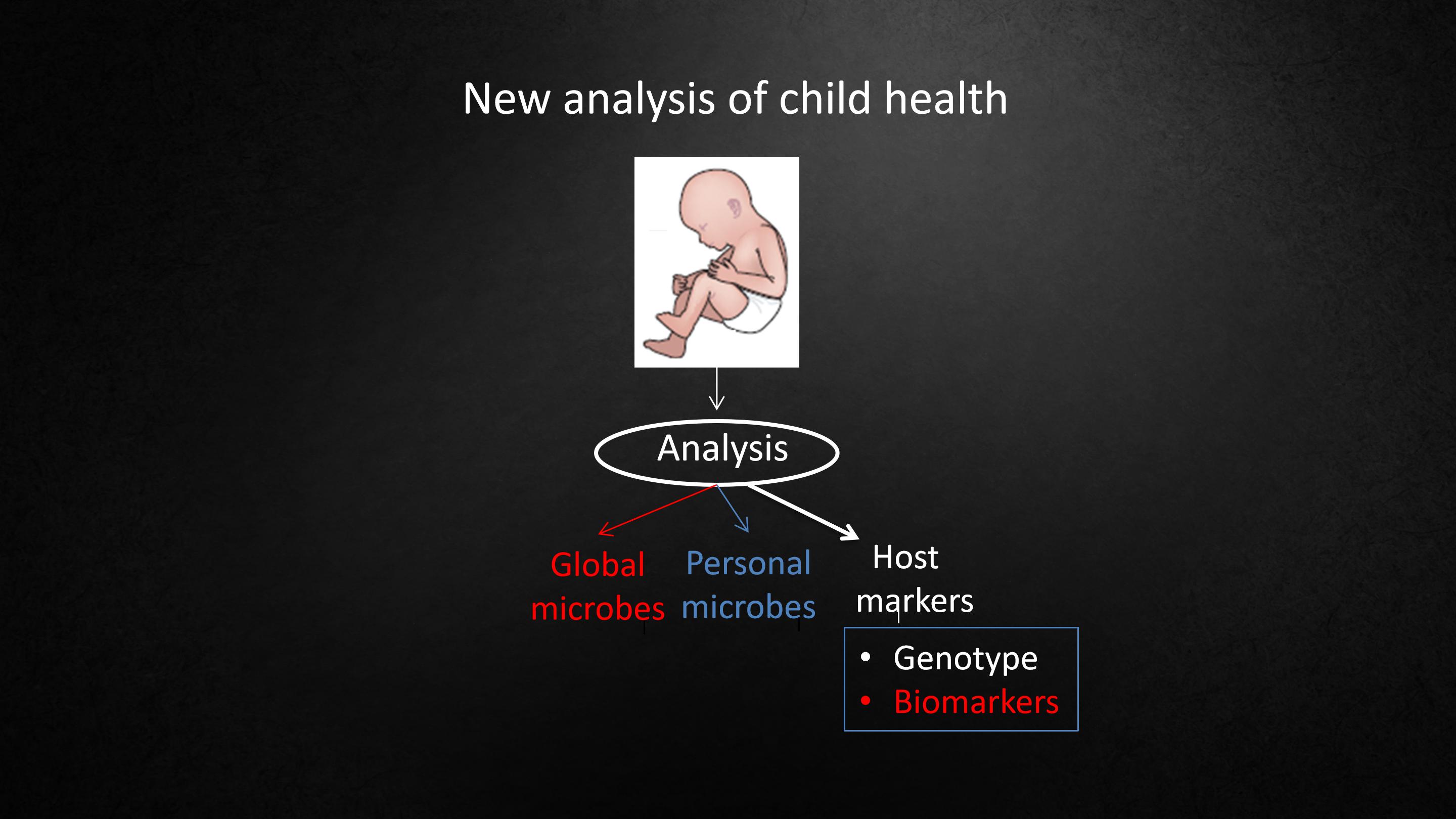
So I think that the doctors of the future, when they examine a baby, are going to examine the baby's diaper.
And they're going to ask, does this baby have all the microbes that they should have? The global microbes that every baby should have? Or certain personal microbes that that particular baby should have based on who that baby is and what's their genetics?
我想,当未来的医生检查婴儿时,应该要检查婴儿的尿布。
他们会问,这个婴儿拥有所有他应有的微生物吗?每个婴儿应有的所有微生物都有了吗?或者是基于婴儿是谁以及他们的遗传而必须有的某些个体化微生物?
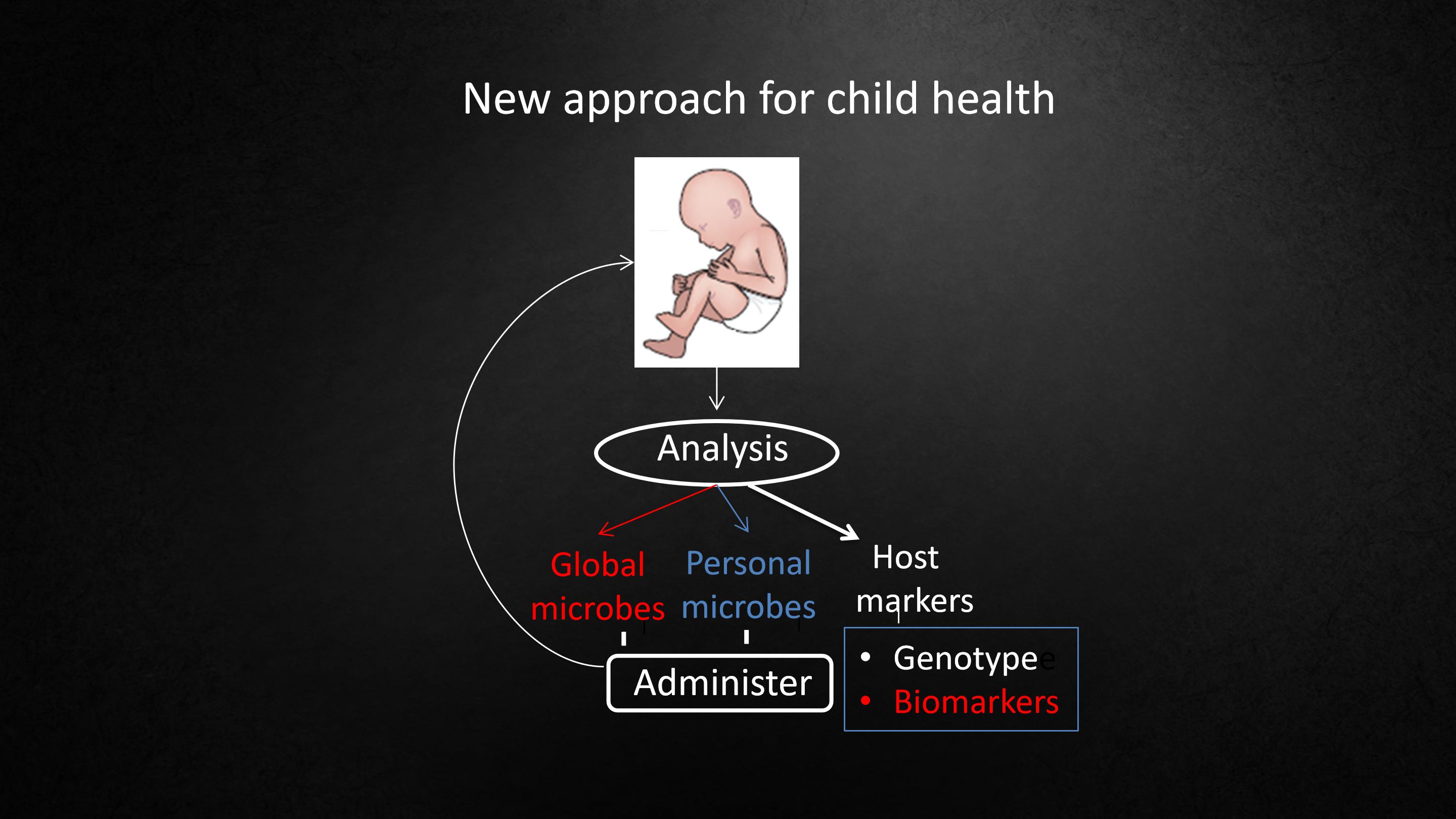
And if the baby doesn't have those microbes, I'm thinking the next generation of doctors are going to give those microbes back to the baby to try to restore their health, and to study what's going to be the effect on the baby.
如果婴儿没有这些微生物,我认为以后的医生应该把这些微生物移植回婴儿体内,以努力恢复他们的健康,并研究这会对婴儿产生什么影响。
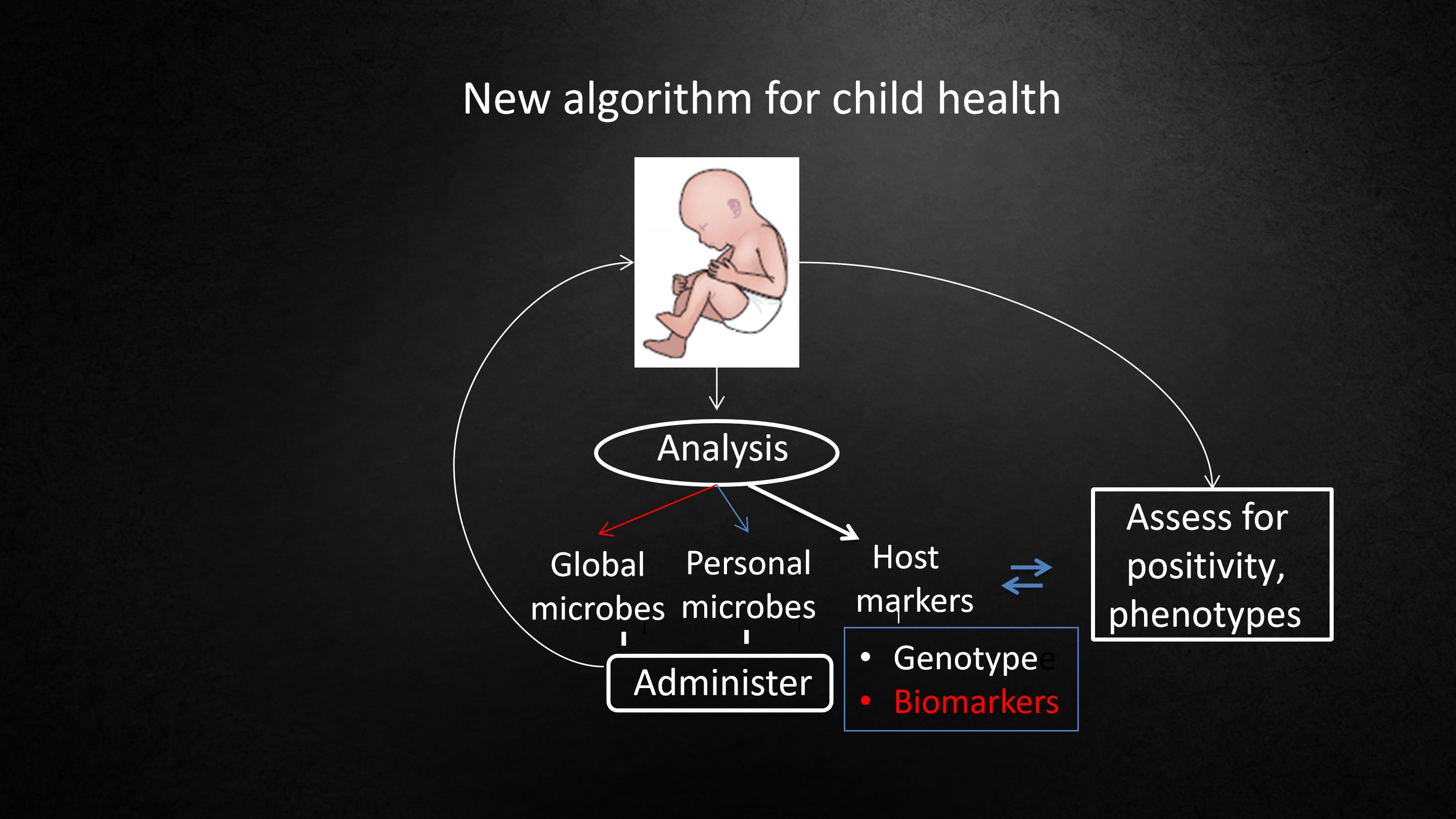
Is this going to make them better or not?
This is what I think the medicine of the future is going to look like.
这是否会让他们变得更好?
这就是我所认为未来的医学的样子。

So what's my advice for mothers in China, mothers everywhere in the world?
We need to reduce antibiotic exposures unless they are medically necessary, unless the doctor says this child, this person must have an antibiotic.
We need to avoid antibiotic taking of young girls and young women unless necessary.
Avoid taking antibiotics in pregnancy unless necessary.
Don't have a cesarean section unless it has to be done.
Don't give your baby antibiotics unless it has to be done.
Babies should be nursed as long as possible.
We should avoid foods that have antibiotics in them.
We should avoid drinking water that contains antibiotics.
This is a lot to think about, but I'm very happy for everyone's attention.
Thank you very much.
我对中国以及全世界的妈妈们有什么建议呢?
我们要减少接触抗生素,除非这是医疗所必须,除非医生说这个孩子,这个人必须使用抗生素。
我们要避免年轻女孩和妇女使用抗生素,除非必要。
避免孕期服用抗生素,除非必要。
不要剖腹产,除非必要。
不要给你的宝宝使用抗生素,除非必要。
婴儿应接受尽可能长的母乳喂养。
我们应该避免食用含有抗生素的食物。
我们应该避免饮用含有抗生素的水。
这需要考虑很多,但我对大家的关注感到很高兴。
十分感谢大家。
(全文结束)


